Hepatobiliary Surgery — MCQs

On this page
Which of the following is FALSE regarding hepatic adenoma?
Which of the following clinical situations is associated with an increase in predominantly conjugated ("direct") bilirubin?
What is the most common complication after ERCP?
A 30-year-old female presented with pain in the right upper quadrant of the abdomen after 4 days of cholecystectomy. On USG, it showed a significant collection in RUQ. What will you do further?
A 46-year-old male had a tumor in his left lobe of liver, so left sided hemi hepatectomy was planned. Which of the following segments of the liver will be resected in this procedure?
Which of the following is the classical triad of acute cholangitis?
A 55-year-old diabetic male develops sudden-onset severe abdominal pain 3 days after an uncomplicated laparoscopic cholecystectomy. Examination reveals peritonitis with guarding and rigidity. Abdominal X-ray shows free air under the diaphragm. What is the most likely diagnosis?
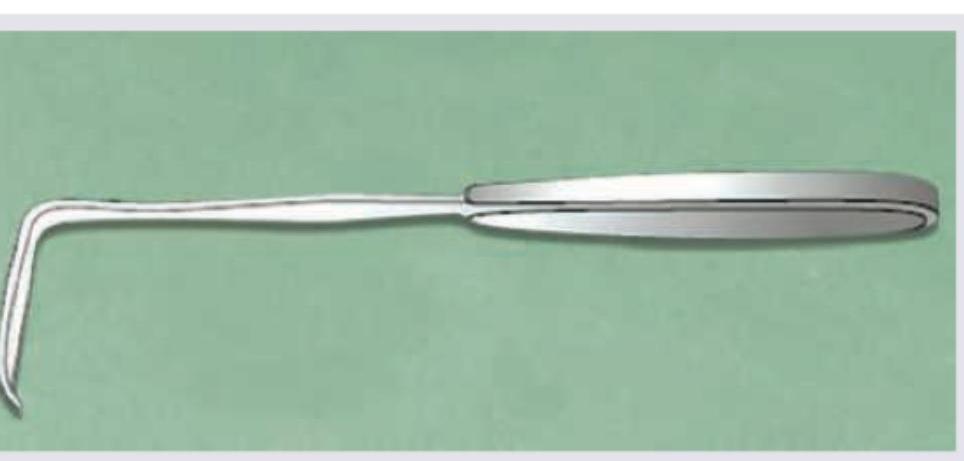
Identify the instrument in the image:
A 25-year-old shepherd presents with dragging discomfort in right hypochondrium and on examination shows presence of enlarged liver 5 cm below costal margins. The probable diagnosis is:
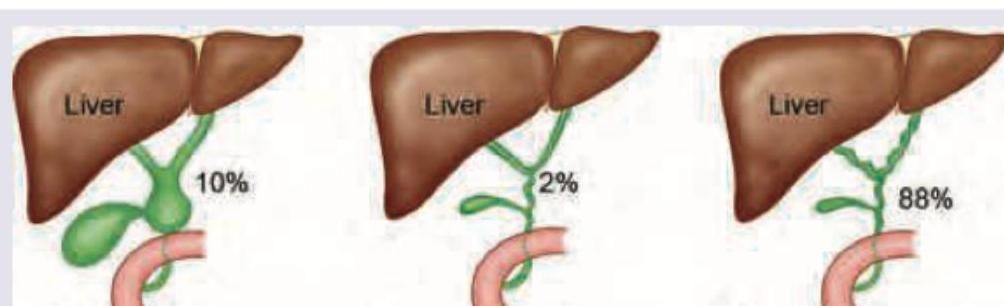
Which of the following is the most common variety of biliary tree: (Recent NEET Pattern 2016-17)
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
