Hepatobiliary Surgery — MCQs

On this page
Which classification is used to divide the liver into segments?
Which of the following statements regarding gall bladder stones is FALSE?
A 30-year-old patient presents with a 5-day history of pain in the right hypochondrium. Examination reveals a soft, tender liver and intercostal tenderness. The patient experiences catching of breath on inspiration and a non-productive cough. Lung fields are clear on auscultation. The patient appears pale and emaciated. What is the probable diagnosis?
Charcot's triad includes which of the following?
What is the preferred treatment for a hydatid cyst?
A 30-year-old patient complains of abdominal pain for 5 days, with a similar history in the recent past. On examination, localized tenderness in the right upper quadrant on deep palpation is observed, along with slight yellowish discoloration of the skin. Ultrasonography reveals certain findings. If this patient had associated gallstones, which of the following would be the most likely diagnosis?
A patient with cholangitis underwent surgical intervention. The investigation shown in the post-operative period on the 10th day is:
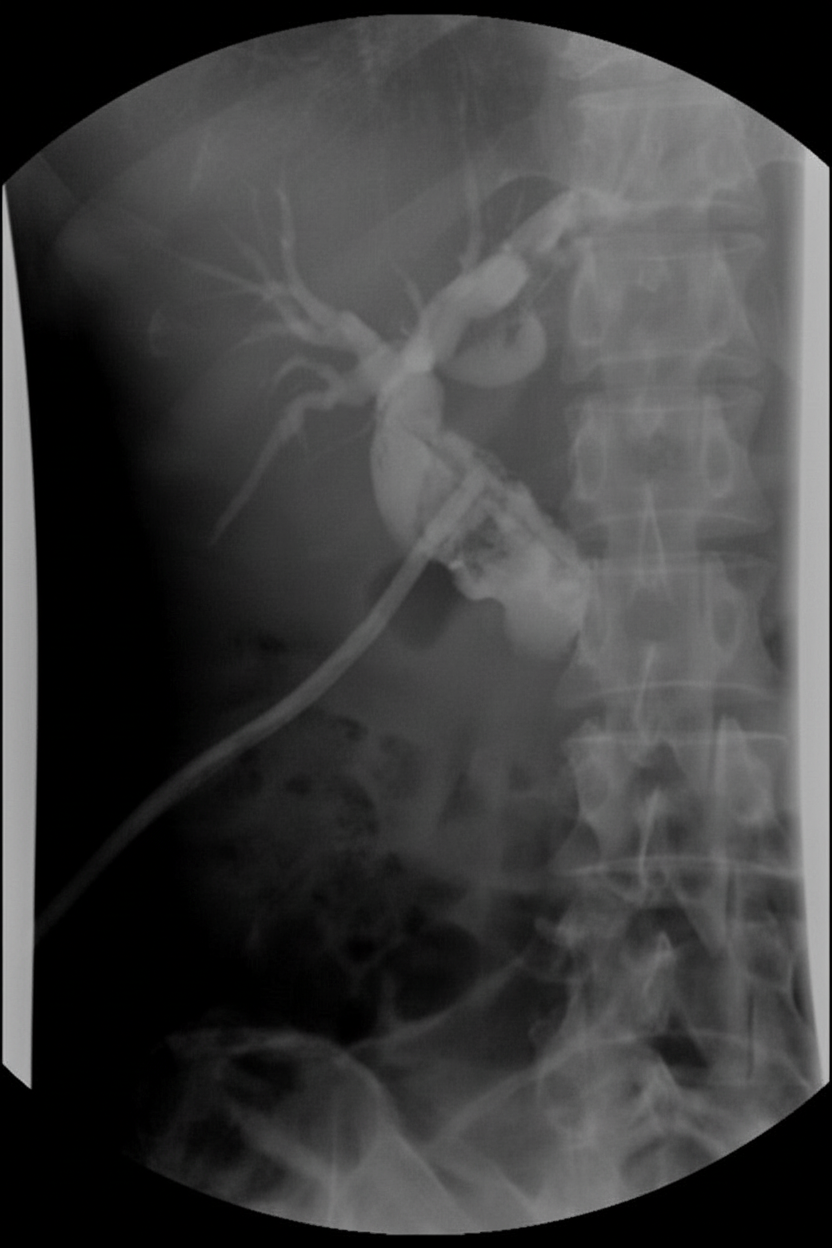
A 70-year-old male presents with complaints of fatigue and jaundice. There is no history of alcohol or liver disease. The liver and spleen are nonpalpable. He has a normocytic, normochromic anemia. What is the first step in the evaluation of this patient?
Which of the following statements about cholangiocarcinoma is false?
Which of the following statements about gall stones is true?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
