Hepatobiliary Surgery — MCQs

On this page
What is the treatment of choice for carcinoma of the head of the pancreas?
Which of the following can be a complication of gallstones?
Which of the following is NOT a criterion for non-resectability in hilar cholangiocarcinoma?
Which of the following constitutes Charcot's triad?
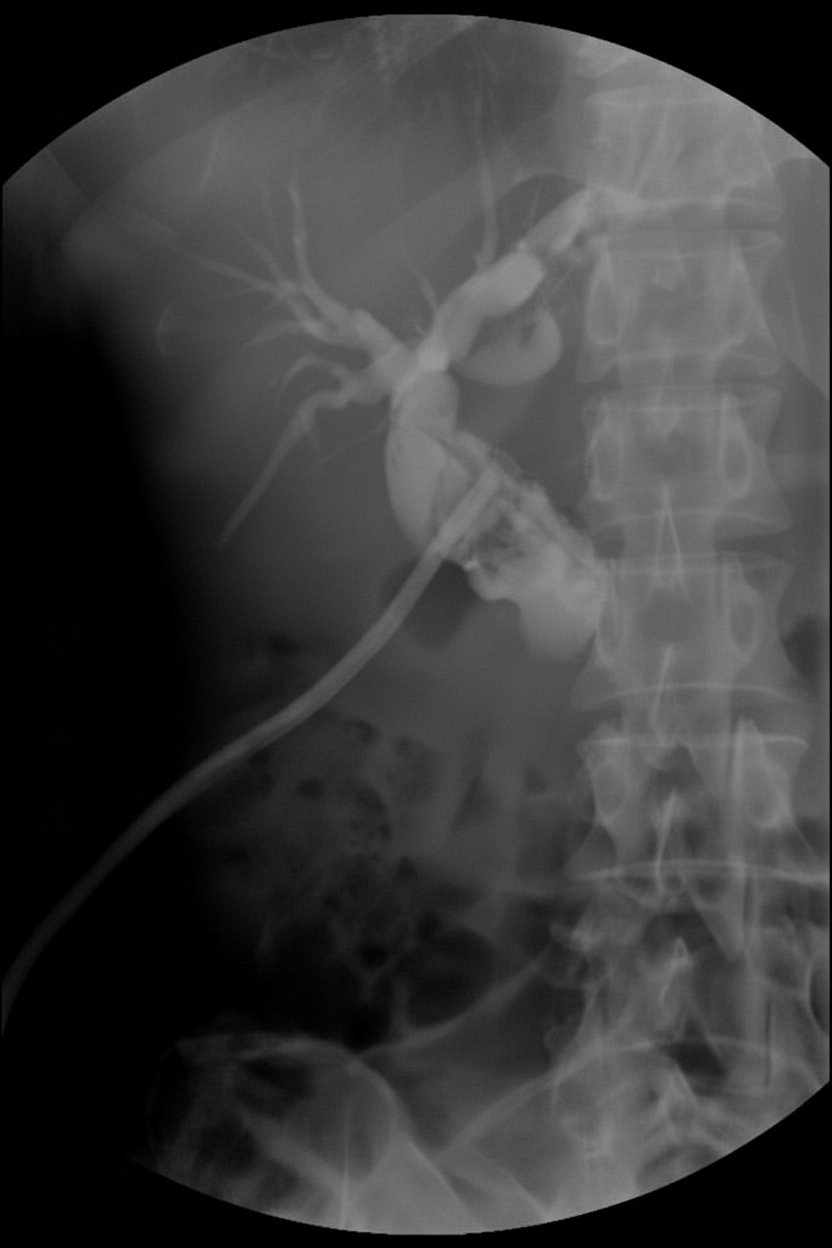
This procedure is performed in which of the following conditions?
Extended cholecystectomy includes removal of all except:
What is the PAIR technique for the treatment of hydatid disease of the liver?
Which condition is characterized by sclerosis of the bile duct?
A 45-year-old female presents with symptoms of acute cholecystitis. Ultrasound shows a solitary gallstone measuring 1.5 cm. Symptoms are controlled with medical management. Which of the following is the next most appropriate step in the management of this patient?
What is the treatment of choice for silent stones in the gallbladder?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
