Hepatobiliary Surgery — MCQs

On this page
Which of the following tumors is typically found incidentally during investigations?
Which of the following is not a major high-risk factor for cholangiocarcinoma?
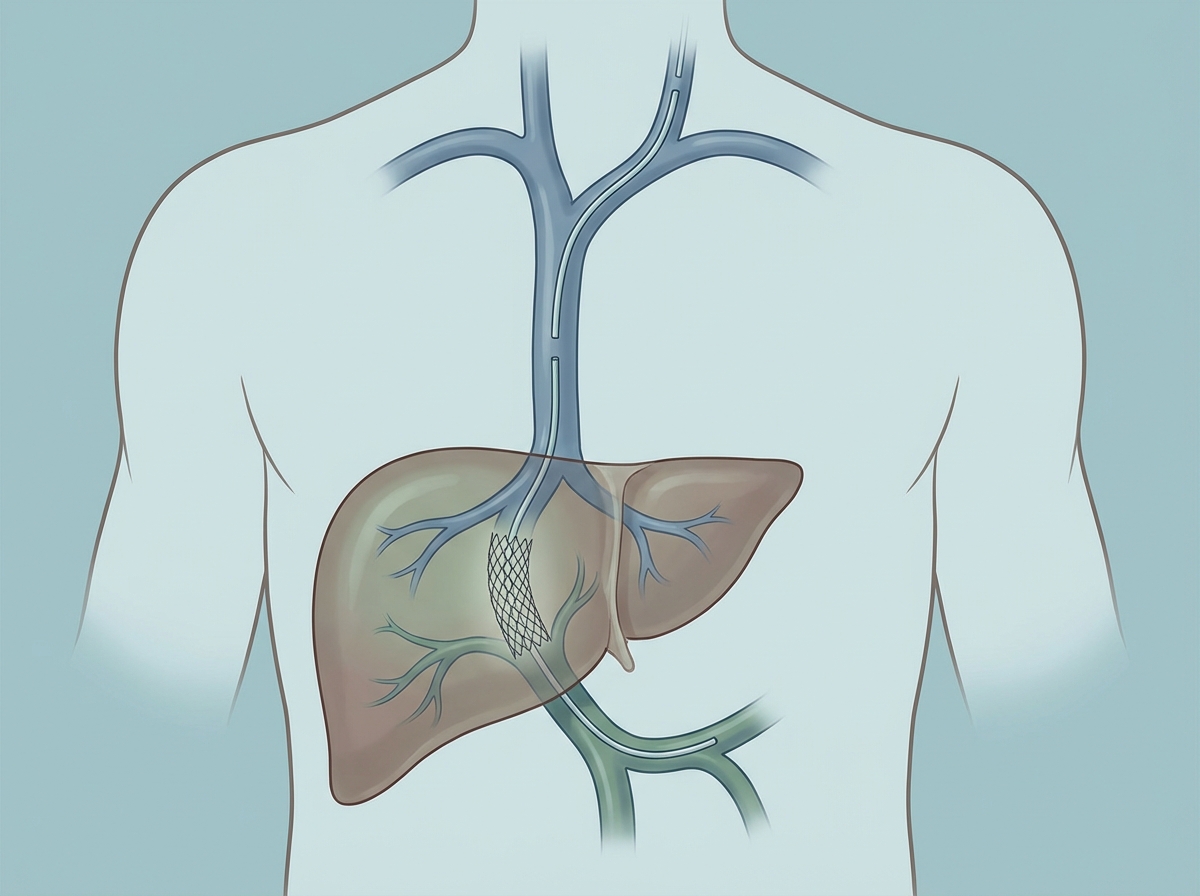
Which of the following is the most common complication of this procedure?
What is the most common type of gallbladder carcinoma associated with gallstones?
What incision approach is used for a mesocaval shunt?
Which of the following originates at the hilum of the liver?
What is Mirrizi syndrome?
All of the following are known predisposing factors for cholangiocarcinoma except:
Which of the following types of hydatid cyst denotes a complicated cyst?
Contraindications for resection in cholangiocarcinoma include all except:
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
