Hepatobiliary Surgery — MCQs

On this page
Which of the following is FALSE about brown pigment stones?
What is the approximate association of choledocholithiasis in patients with cholelithiasis?
Which of the following is NOT a risk factor for malignant change in an asymptomatic patient with a gallbladder polyp identified on ultrasound?
Courvoisier's law is related to which of the following?
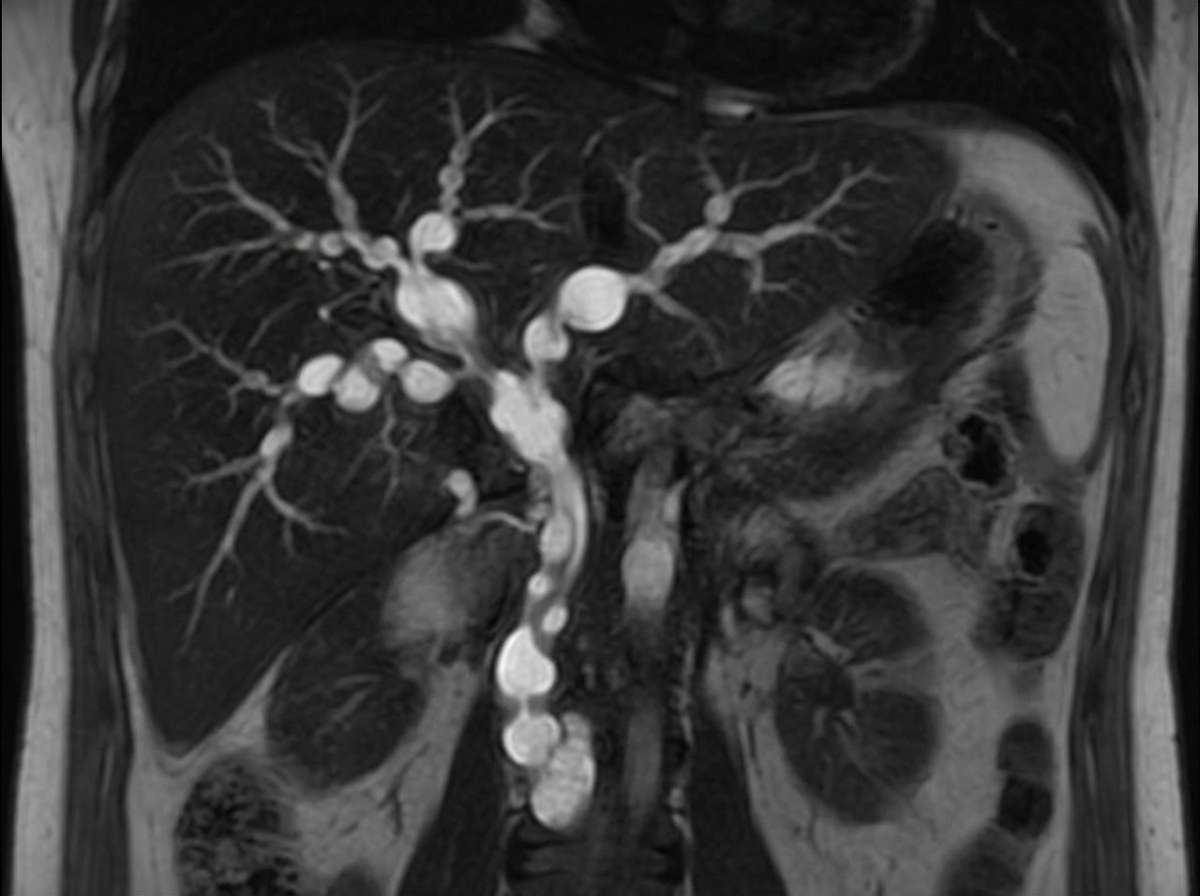
A 45-year-old male presented with recurrent attacks of cholangitis. MRCP and ERCP findings are suggestive of this condition. What is the treatment of choice for this condition?
According to Pugh's classification, moderate to severe hepatic insufficiency is managed by which of the following?
What is the most common cause of hemobilia?
Amoebic liver abscess ruptures most commonly into which cavity?
Which of the following is a characteristic feature of periampullary carcinoma?
Bleeding adjacent to the Triangle of Calot should be controlled by which method?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
