Hepatobiliary Surgery — MCQs

On this page
Charcot's triad includes all of the following except?
Which of the following is NOT true about the triad of hemobilia?
Normal portal vein pressure is:
What is the most important hepatic function to consider after hepatic resection?
Which of the following is a non-selective shunt?
Which of the following is included in the Chilaiditi's sign criteria?
Bile duct injury is detected after 72 hours of surgery. What is the treatment option?
The following is a feature of:
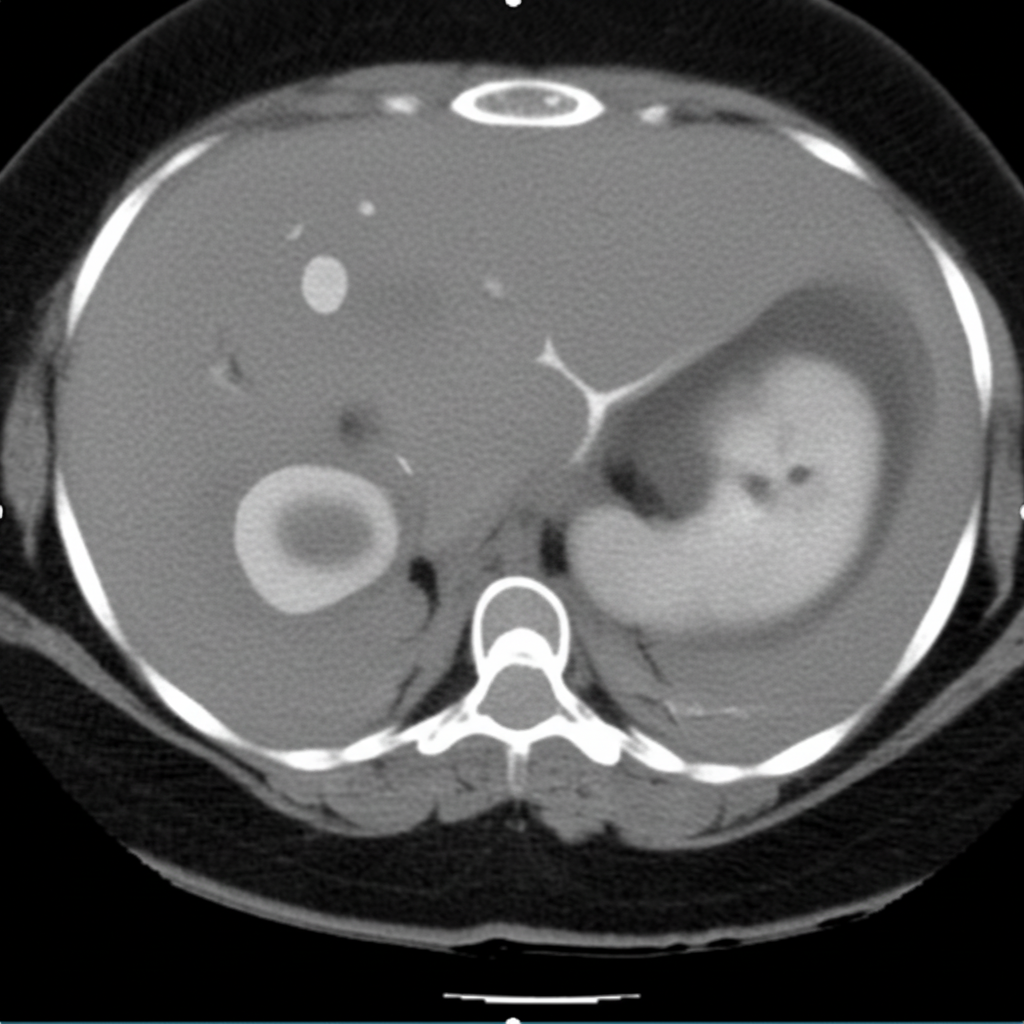
What is a Klatskin tumor?
What is the preferred shunt procedure in a patient with portal hypertension who has acceptable operative risk and adequate liver function?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
