Hepatobiliary Surgery — MCQs

On this page
What is the most common cause of hemobilia?
Tokyo guidelines are used to assess the severity of which condition?
What is the most appropriate treatment for gallbladder carcinoma with invasion of perimuscular connective tissue, diagnosed after laparoscopic cholecystectomy?
Which of the following is NOT true regarding cholangitis?
Acalculous cholecystitis is most commonly seen in which of the following conditions?
What is the indication for medical treatment of gallstones in the A/E setting?
What is the preferred method of removal for a 3cm stone in the cystic duct?
What is the most common cause of suppurative cholangitis?
A 50-year-old chronic diabetic presents with severe abdominal pain, nausea, vomiting, and fever. Abdominal imaging shows [findings]. What is the next best step in managing this patient?
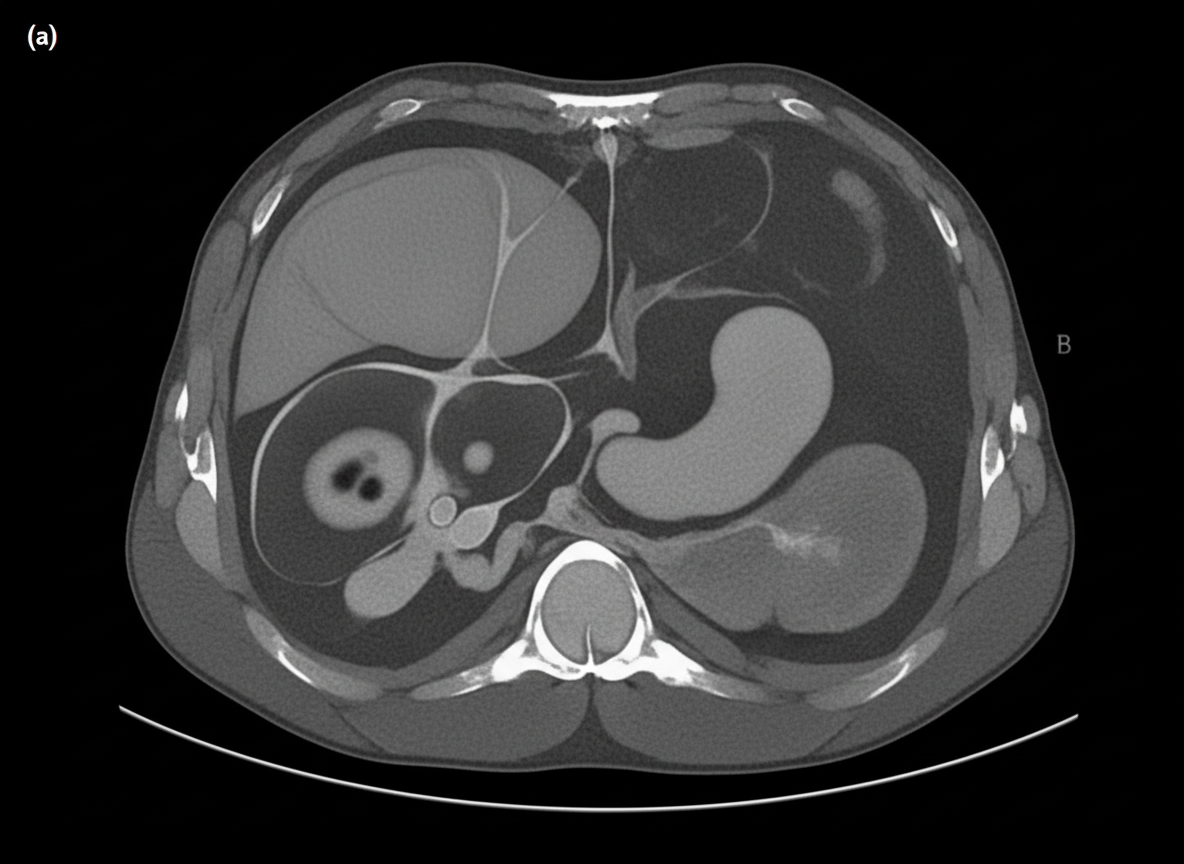
Which of the following is NOT true about Todani's modification of the Alonso-Lej classification?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
