Hepatobiliary Surgery — MCQs

On this page
According to Couinaud's classification, how many lobes are present in the liver?
Which of the following is NOT a risk factor for malignant transformation in an asymptomatic patient with a gall bladder polyp identified on ultrasound?
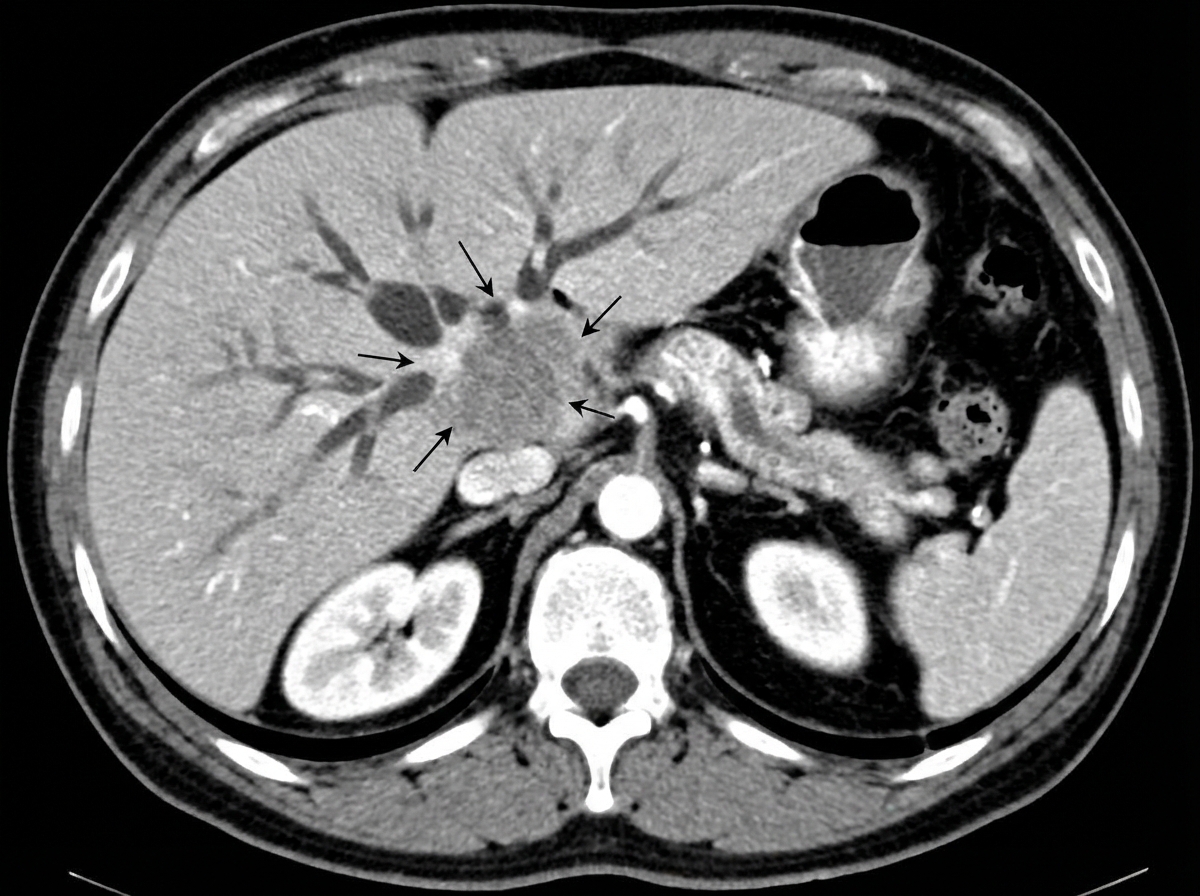
A 70-year-old male presented with progressive jaundice for 6 weeks, fever, pruritis along with abdominal pain and significant weight loss. Lab findings reveal total serum bilirubin of 22 mg/dL, minimally elevated SGOT/SGPT, and increased alkaline phosphatase. A CT abdomen and ERCP were performed. What is the most common site of this pathology?
Which of the following are included in the Child criteria?
A patient presents with abdominal pain, jaundice, and melena. What is the most likely diagnosis?
A 50-year-old man presents with a one-week history of fever and abdominal pain. An abdominal ultrasound revealed a hypoechoic liver lesion, and a CECT was performed for characterization. Which of the following statements regarding the lesion is false?
Okuda staging for HCC includes all except?
Which of the following is a criterion for assessing the prognosis of a portosystemic shunt?
What is the ideal treatment for stenosis of the sphincter of Oddi?
Which of the following is an indication for surgical removal of polypoid lesions of the gallbladder?
Practice by Chapter
Liver Anatomy and Physiology
Practice Questions
Benign Liver Lesions
Practice Questions
Liver Abscess
Practice Questions
Hepatocellular Carcinoma
Practice Questions
Metastatic Liver Disease
Practice Questions
Cirrhosis and Portal Hypertension
Practice Questions
Liver Trauma
Practice Questions
Cholelithiasis and Cholecystitis
Practice Questions
Choledocholithiasis
Practice Questions
Biliary Tract Tumors
Practice Questions
ERCP and Its Complications
Practice Questions
Liver Transplantation Basics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
