ERCP and Its Complications — MCQs

Cholestasis may lead to the following complications except:
Which of the following is a common cause of acute pancreatitis?
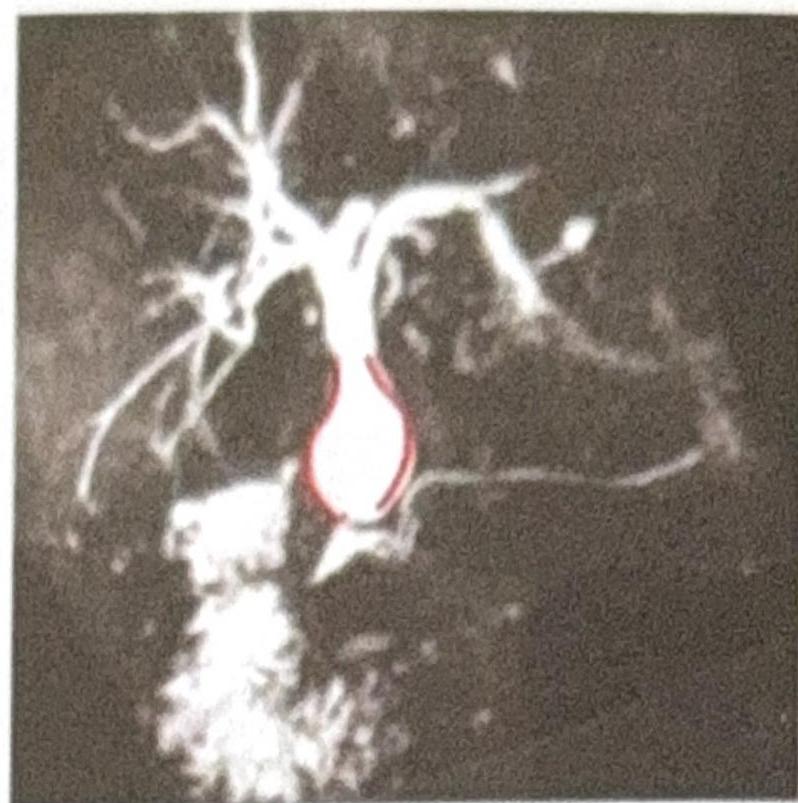
What condition does the MRCP (Magnetic Resonance Cholangiopancreatography) image indicate?
Which intervention should Nurse Bryan include in the care plan for Pierre, a client diagnosed with acute pancreatitis under his care?
Which of the following is a complication of gallstones?
What is the definitive treatment for gallstone-induced pancreatitis?
On the 5th postoperative day after laparoscopic cholecystectomy, a 50-year-old lady presented with right upper quadrant pain, fever, and a 12-cm subhepatic collection on CT. What is the best management option for this patient?
Which of the following is NOT a primary function of histamine antagonists as a drug class?
A patient with multiple gallstones shows 8 mm dilation and has 4 stones in the common bile duct (CBD). What is the best treatment modality?
The percutaneous PAIR therapy used in the treatment of uncomplicated hepatic hydatid cyst can be associated with the following complications, except
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
