Head and Neck Surgery — MCQs

On this page
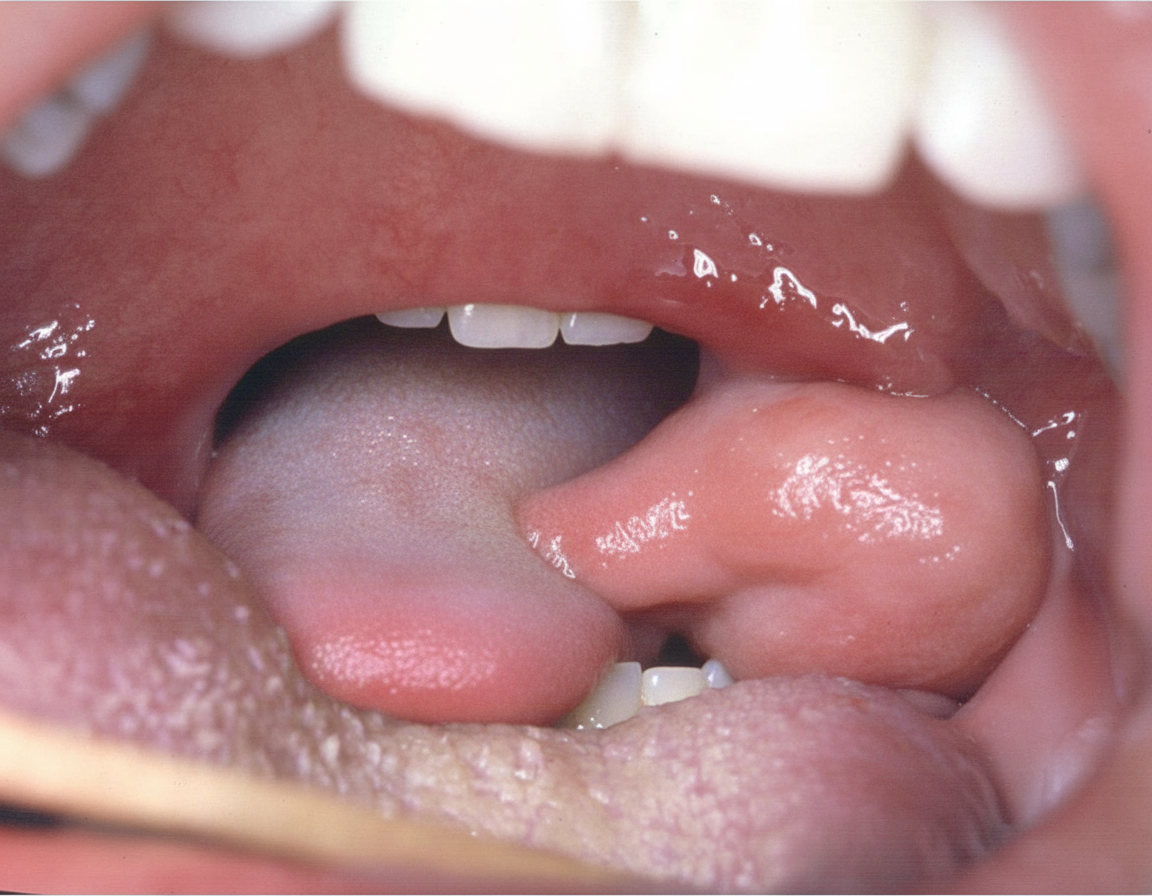
What is the most common organism that causes the following condition?
How many Champy's osteosynthesis lines exist behind and in front of the mental foramen?
Which of the following statements about cleft palate is incorrect?
Excessive blood loss during mandibulectomy can be prevented by all of the following except?
All of the following are indications for CT scan in a head-injured patient except?
The propensity of recurrence after surgical intervention is the least in which of the following conditions?
Which of the following is characteristic of carcinoma of the tongue?
A thyroglossal cyst is most often located:
An 85-year-old ventilator-dependent male was endotracheally intubated 10 days ago. He remains unresponsive and is not a candidate for early extubation. The intensive care unit (ICU) attending elects to perform tracheostomy at the bedside. During the procedure, copious dark blood is encountered. This is most likely due to transection of which of the following?
A 56-year-old smoker presented with swelling over the parotid region. Histology shows papillary structures composed of granular eosinophilic cells, cystic changes, and mature lymphocytic infiltration, which is pathognomonic of Warthin tumor. What is the treatment of choice for Warthin tumor?
Practice by Chapter
Salivary Gland Diseases
Practice Questions
Thyroid Gland Disorders
Practice Questions
Parathyroid Gland Disorders
Practice Questions
Neck Masses Evaluation
Practice Questions
Oral Cavity Lesions
Practice Questions
Laryngeal Disorders
Practice Questions
Head and Neck Cancer
Practice Questions
Reconstructive Techniques in Head and Neck Surgery
Practice Questions
Surgical Management of Sleep Apnea
Practice Questions
Airway Management in Head and Neck Surgery
Practice Questions
Surgical Approaches to the Neck
Practice Questions
Neck Dissection Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
