Head and Neck Surgery — MCQs

On this page
A patient presents with chronic sinusitis that is unresponsive to medical therapy. A CT scan reveals mucosal thickening and obstruction at the osteomeatal complex. What is the next best step in management?
A 55-year-old female presents with a rapidly enlarging neck mass and stridor. Fine needle aspiration is inconclusive. What is the most appropriate next step?
A 50-year-old female presents with a mass in the floor of the mouth. On examination, the mass is firm, non-tender, and there is no cervical lymphadenopathy. What is the most likely diagnosis?
A surgeon accidentally lacerates a nerve close to the angle of the mandible during a submandibular gland excision. Which nerve is at risk in this situation?
A patient with a pituitary tumor undergoes transsphenoidal surgery for tumor resection. Which anatomical structure serves as the surgical access route in this procedure?
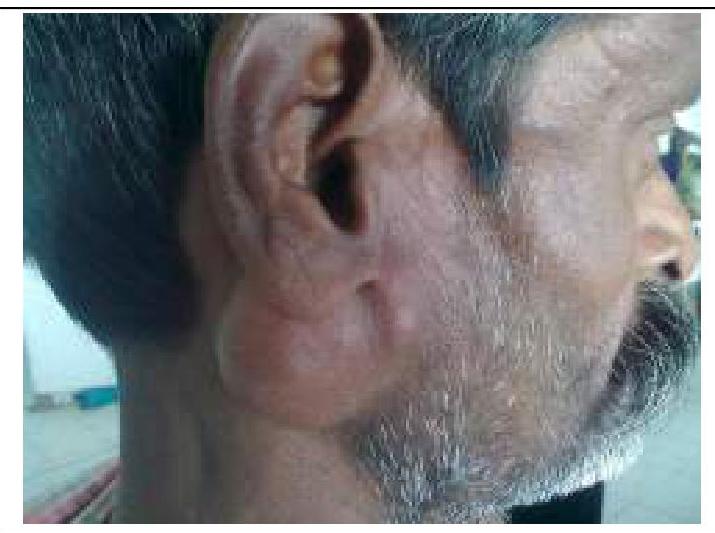
A 60-year-old man presents with painless, progressive enlargement of the parotid gland. What is the most likely diagnosis?
A middle-aged man with a swelling over the neck since childhood with the overlying skin not intact which had a bag or worm-like appearance with a black spot in the middle. What will be the diagnosis?
What is the most likely diagnosis for the parotid mass with mixed consistency shown in the image?
Preferred treatment for oral tongue carcinoma which infiltrates the local cortical bone is -
Burr hole is done for -
Practice by Chapter
Salivary Gland Diseases
Practice Questions
Thyroid Gland Disorders
Practice Questions
Parathyroid Gland Disorders
Practice Questions
Neck Masses Evaluation
Practice Questions
Oral Cavity Lesions
Practice Questions
Laryngeal Disorders
Practice Questions
Head and Neck Cancer
Practice Questions
Reconstructive Techniques in Head and Neck Surgery
Practice Questions
Surgical Management of Sleep Apnea
Practice Questions
Airway Management in Head and Neck Surgery
Practice Questions
Surgical Approaches to the Neck
Practice Questions
Neck Dissection Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
