Head and Neck Surgery — MCQs

On this page
Which structure is damaged in a high tracheostomy?
Facial nerve injury occurs during parotid surgery. What is the best management?
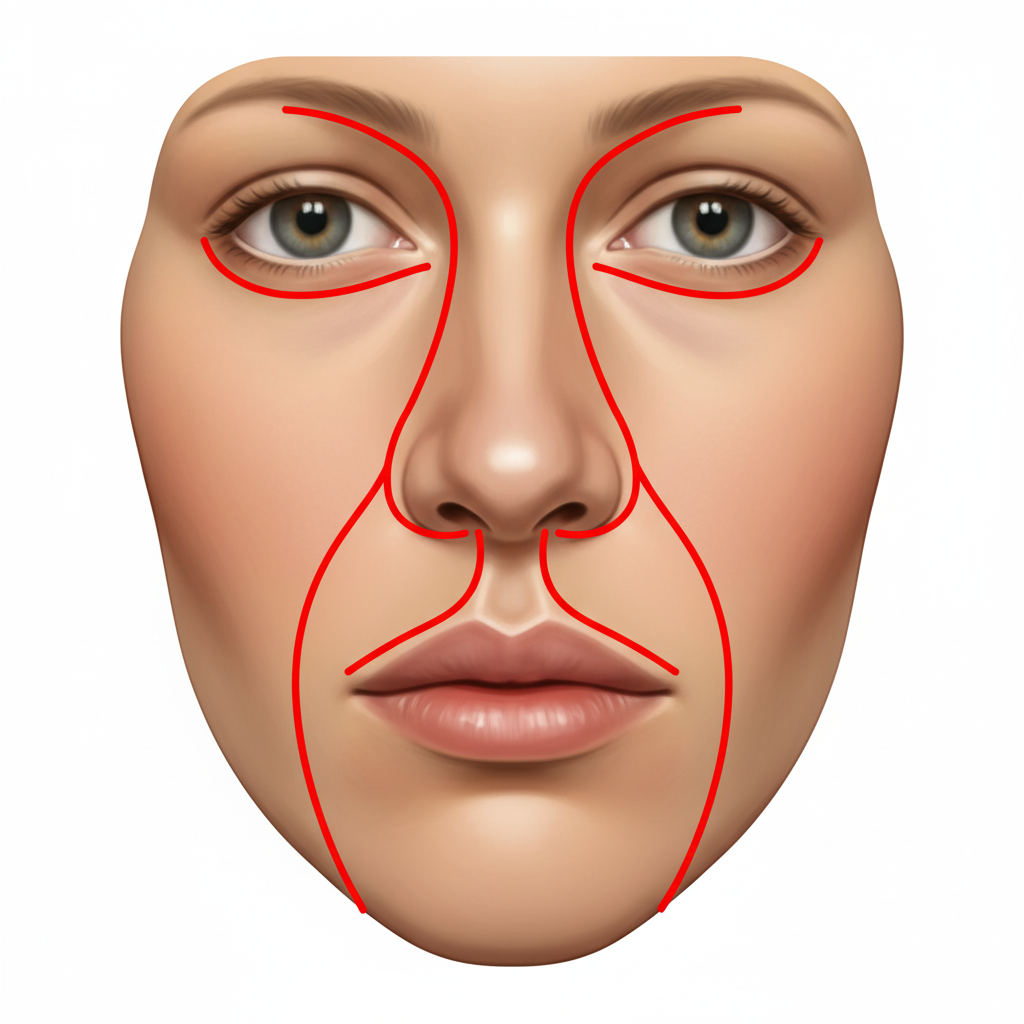
What is the name of the incision shown below?
A 21-year-old woman presents with a 3 cm node in the lower deep cervical chain on the left. Biopsy reveals normal thyroid tissue within a lymph node. What is the most likely diagnosis?
A female presented with a severe headache of sudden onset. On CT scan, a diagnosis of subarachnoid hemorrhage is made. What is the most common cause of subarachnoid hemorrhage?
What is true about carotid body tumors?
A 58-year-old woman undergoes excision biopsy of a tumor in the left posterior triangle of her neck. Histology suggests that this is a metastatic cancer. What is the most likely site of the primary tumor?
A 70-year-old male presented with an asymptomatic white patch on the oral cavity following the application of a denture. What is the treatment of choice?
Which of the following structures is preserved in a functional radical dissection of the neck, except?
A 4-year-old girl presenting with a painless, mobile, cystic swelling in the midline of her neck, located just below the hyoid bone, is scheduled for tonsillectomy. The swelling measures 2x1x1 cm. An ultrasound reveals a thick-walled cystic lesion. What is the recommended management?
Practice by Chapter
Salivary Gland Diseases
Practice Questions
Thyroid Gland Disorders
Practice Questions
Parathyroid Gland Disorders
Practice Questions
Neck Masses Evaluation
Practice Questions
Oral Cavity Lesions
Practice Questions
Laryngeal Disorders
Practice Questions
Head and Neck Cancer
Practice Questions
Reconstructive Techniques in Head and Neck Surgery
Practice Questions
Surgical Management of Sleep Apnea
Practice Questions
Airway Management in Head and Neck Surgery
Practice Questions
Surgical Approaches to the Neck
Practice Questions
Neck Dissection Techniques
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
