General Surgery Principles — MCQs

On this page
Which of the following are tension-free inguinal hernia repairs? 1. Stoppa's repair 2. Lichtenstein's repair 3. Laparoscopic TEP repair 4. Desarda's repair.
When the hernia extends between the layers of abdominal wall muscles and not directly through them, it is called
Which of the following is the PRIMARY factor that predisposes to the development of incisional hernia?
Match List-I with List-II and select the correct answer using the code given below the Lists: (Refer to the image for List-I and List-II)
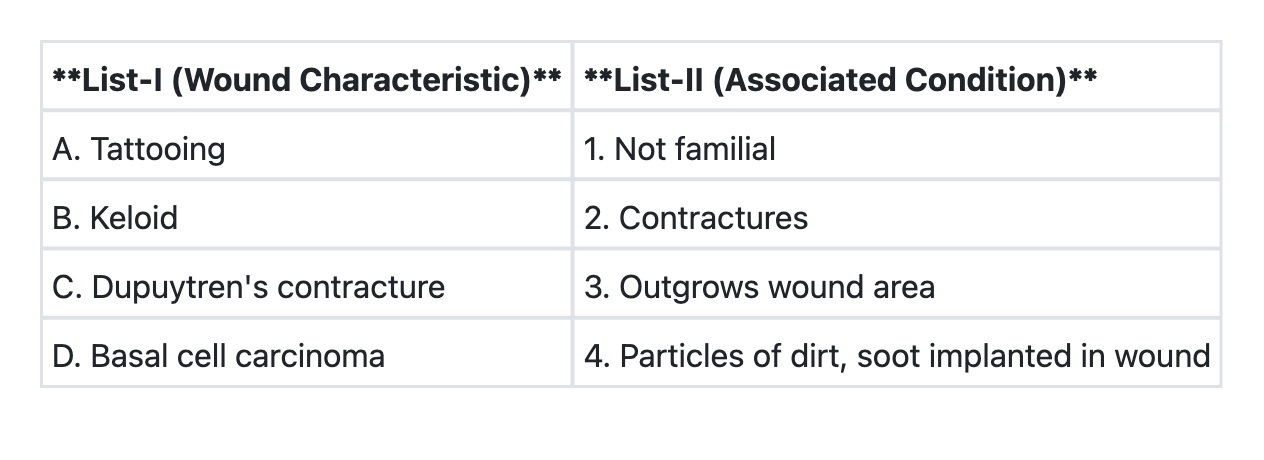
Consider the following statements regarding splenectomy : 1. It corrects anemia in congenital hereditary spherocytosis. 2. Postponed until the age of 4 years if possible. 3. Polyvalent pneumococcal vaccine to be administered to all before the surgery. Which of the statements given above are correct ?
Splenectomy is best indicated for :
Which one of the following nerves is vulnerable to injury while conducting an appendicectomy through the McBurney's incision ?
Splenectomy is indicated in all of the following conditions, except
The term "debridement of the wound" refers to
Tidy wounds inflicted by sharp instruments and containing no devitalised tissues are expected to heal by
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
