General Surgery Principles — MCQs

On this page
Catgut suture is derived from which part of the sheep?
Which of the following is the most commonly used site for Deep Brain Stimulation to reduce the frequency of Parkinsonism symptoms?
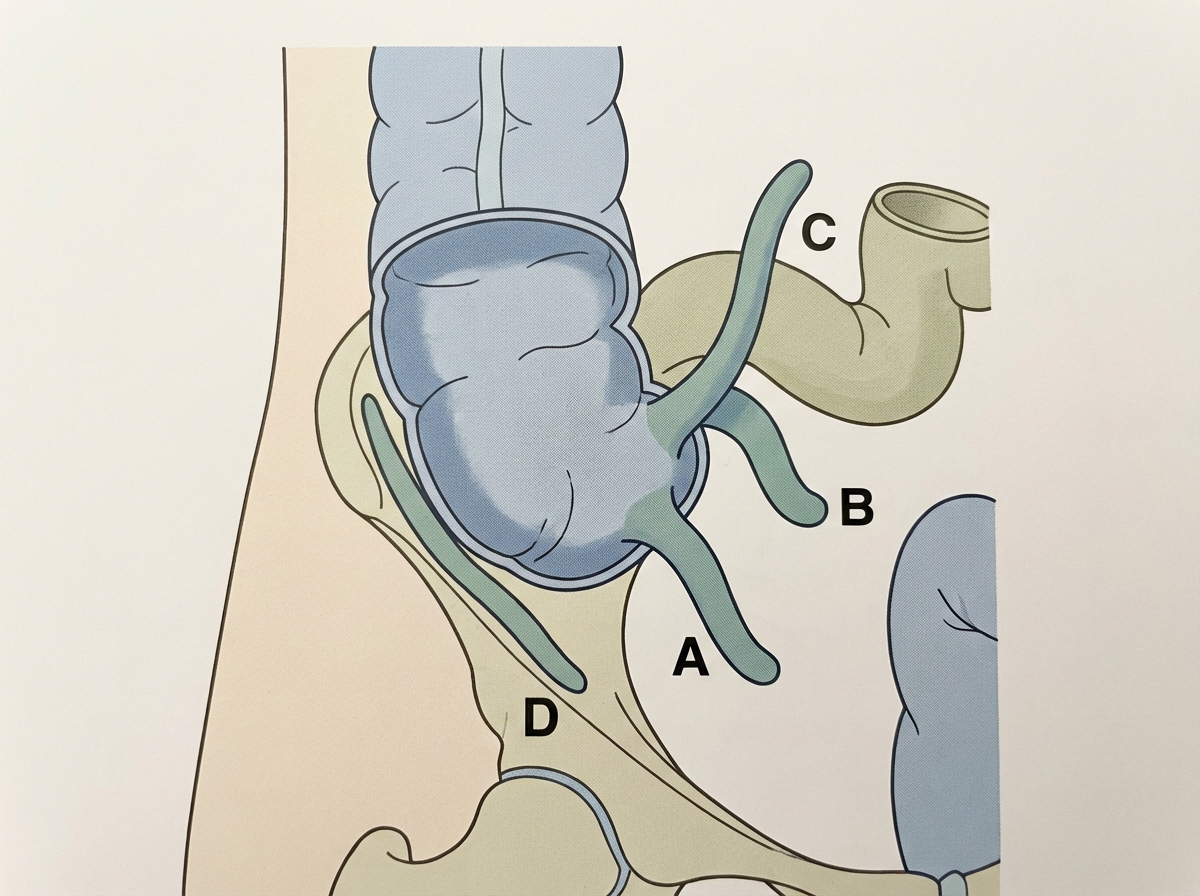
A 20-year-old male patient presented to the ER with complaints of abdominal pain, nausea, and vomiting. The pain was initially peri-umbilical in nature; however, with time, the pain worsened and shifted to the right lower quadrant. On palpating the abdomen, tenderness is present over the right lower quadrant with guarding. The patient is febrile and lab reports show leukocytosis. An emergency laparotomy is planned, and the inflamed organ is identified by the confluence of taenia coli. Which position of the above-mentioned organ is considered to be the most dangerous position?
A 80-year-old male presented with a lung abscess in the left upper zone. What is the best treatment modality?
Spigelian hernia occurs through which anatomical structure?
Post-splenectomy, which of the following infections is not common?
All of the following are true regarding sebaceous cysts EXCEPT:
What is the treatment for bilateral soft tissue undercut?
Which of the following is NOT a differential diagnosis for acute scrotum?
Graft survival for the first 48 hours is primarily due to which of the following?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
