General Surgery Principles — MCQs

On this page
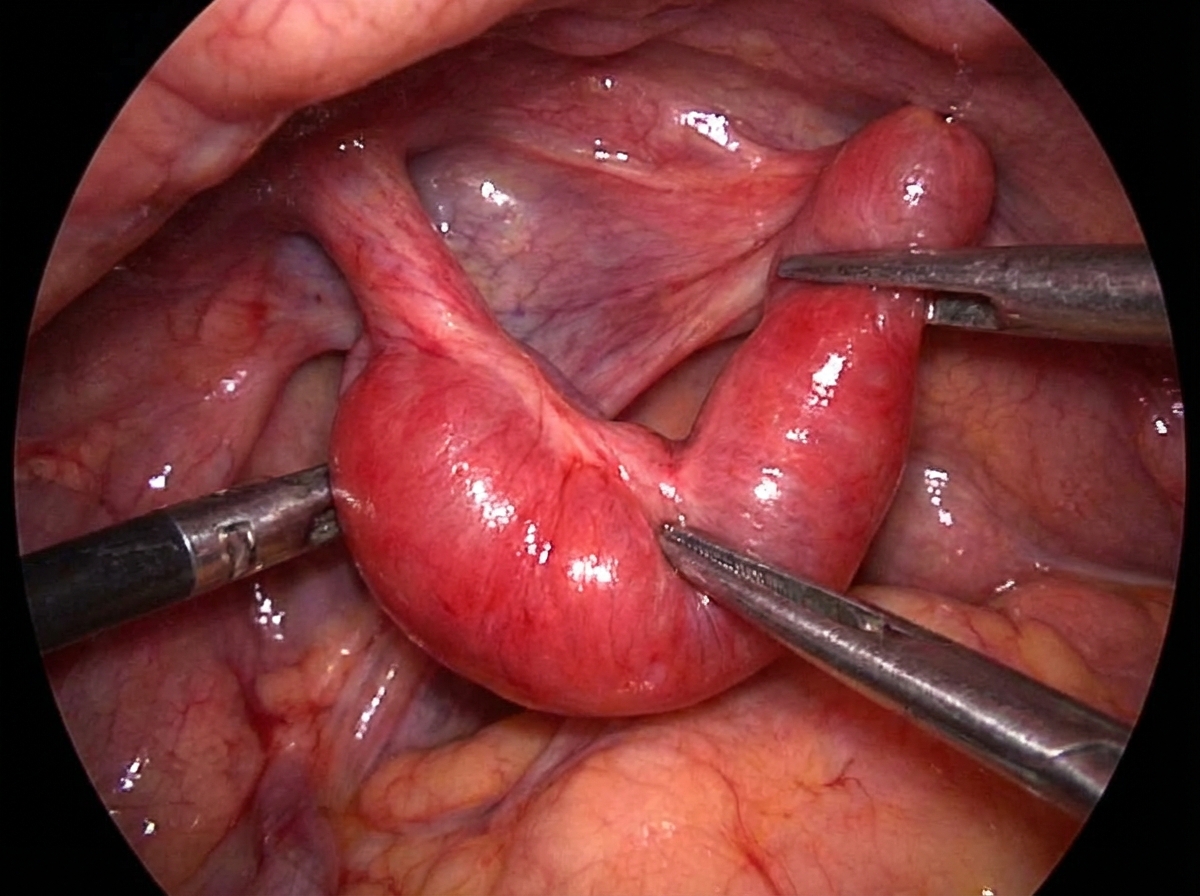
Which scoring system is used to diagnose the condition suggested by the surgical procedure shown?
A lady presented to the emergency department with a stab injury to the left side of the abdomen. She was hemodynamically stable, and a contrast-enhanced CT scan revealed a laceration in the spleen. Laparoscopy was planned; however, the patient's PO2 suddenly dropped as soon as pneumoperitoneum was created. What is the most likely cause?
In a patient recovering from peritonitis, which of the following would be the most characteristic sign of pelvic abscess?
At what age is cleft lip repair commonly performed?
What is a complication of total parenteral nutrition (TPN)?
Which classification best describes the surgical wound for an elective hemicolectomy for carcinoma of the colon?
The Gilbert classification system is used for which type of condition?
Which one of the following does not cause post-splenectomy septicemia?
A 30-year-old obese male patient presents with a complete inguinal hernia. On examination, a doughy consistency is felt with a dull note on percussion. What does this suggest about the contents of the hernia sac?
Which of the following is NOT a premalignant ulcer?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
