General Surgery Principles — MCQs

On this page
Negative pressure dressing is used for which of the following indications?
Hydatid cyst occurs most commonly in which organ?
The provided image is a thyroid scan. Based on the scan, what is the most probable diagnosis?
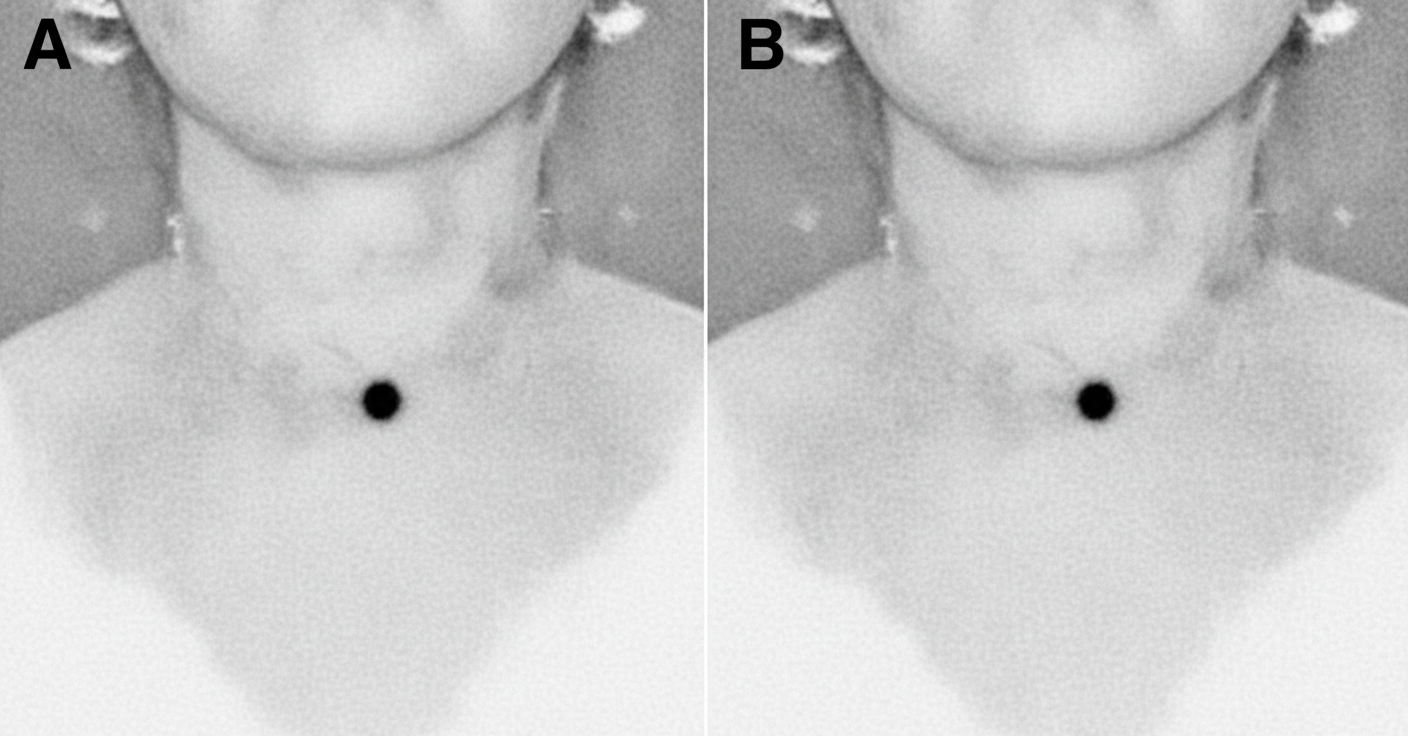
What is a keloid scar?
Reactionary hemorrhage occurs after extraction because of which of the following?
A Grade III wound is considered contaminated if it is:
Which of the following statements about Pilonidal sinus is true?
All of the following are true about hernia surgery except:
In diabetic foot, which type of amputation is contraindicated?
What is the most common complication following hemorrhoidectomy?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
