General Surgery Principles — MCQs

On this page
Basal cell carcinoma spreads primarily by which mechanism?
Who introduced antiseptic surgery?
All of the following are true about Enteral nutrition except:
In which degree of burns is the dermis involved?
Stemmer's sign and buffalo hump are features of which condition?
Which of the following is NOT a proactive approach to prevent unnecessary stress in a surgical patient?
Which of the following statements about hernia is false?
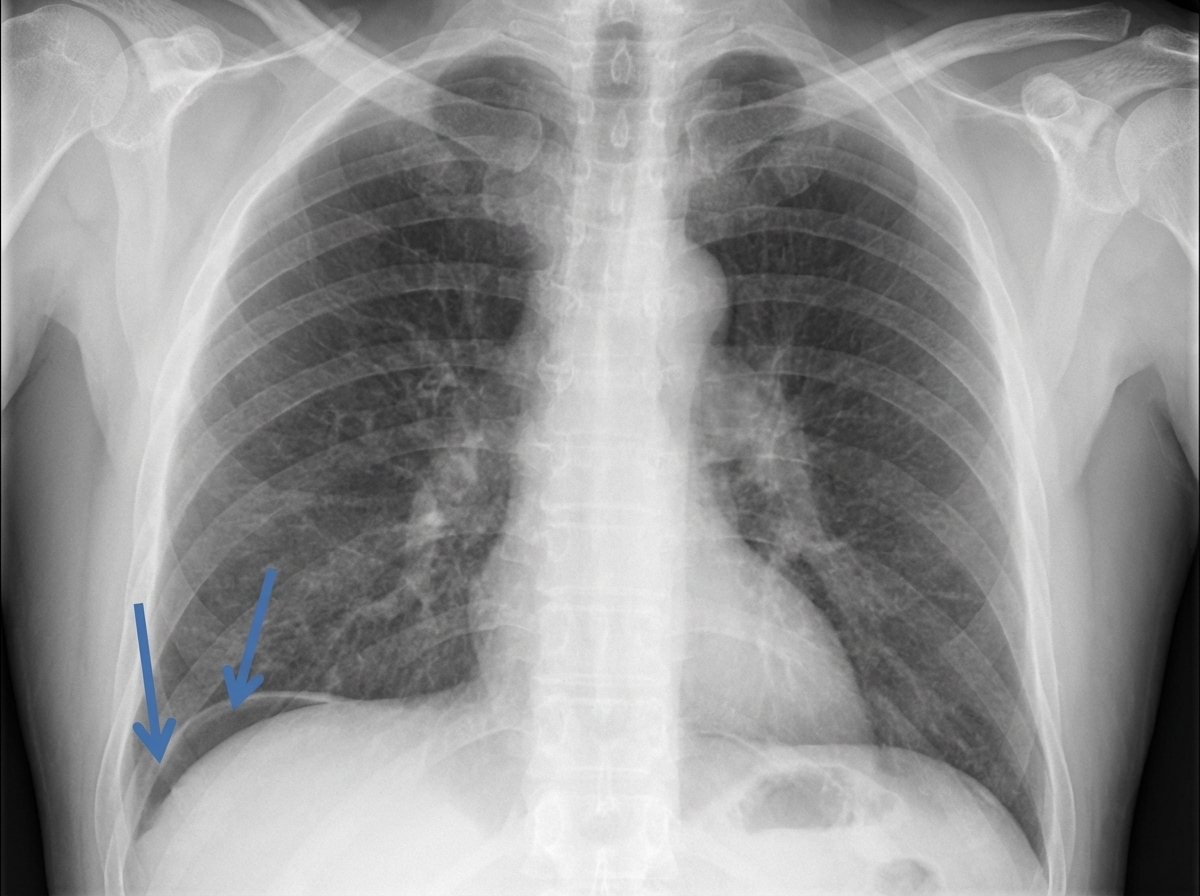
A patient presented to the emergency department with severe abdominal pain. An erect radiograph was performed. Based on the findings, what should be the management?
During a preoperative assessment of the airway, only the hard palate is visible when the patient phonates. What is the grade according to the modified Mallampati test?
Strangulation most commonly occurs in which of the following conditions?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
