General Surgery Principles — MCQs

On this page
This instrument, historically used for opening sinus ostia in sinusitis, has a blunt tip. Surgeons currently use it to drain abscesses in which of the following regions?
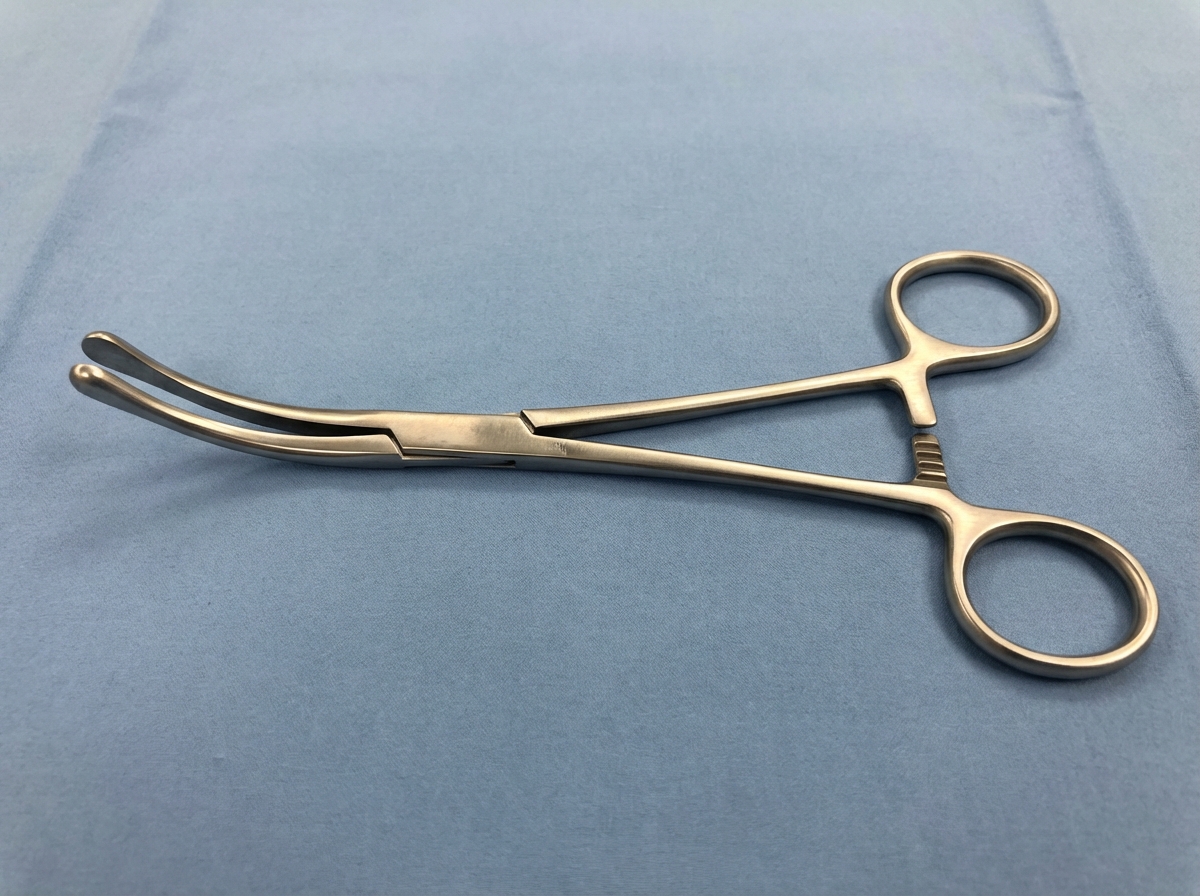
Splenectomy is indicated in:
You are performing a 5-year follow-up on a 43-year-old implant patient. When comparing radiographs, you estimate that there has been almost 0.1 mm loss of bone height around the implant since it was placed. What is indicated?
Amyand's hernia is defined as which of the following?
A patient with Child's C cirrhosis has had repeated episodes of variceal bleeding and ascites. What is the treatment of choice?
What is the treatment of an uncomplicated hydatid cyst in the lung?
What is the treatment of choice for bilateral bony tissue undercut?
Surgical approaches for open thymectomy include all except?
When forceps are utilized for tooth removal, what is the initial direction of force application?
Which of the following is NOT a pro-inflammatory cytokine?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
