General Surgery Principles — MCQs

On this page
All are genetic conditions with increased risk of malignancy except?
Which of the following conditions does not typically present with bleeding per rectum?
What is the most common type of cyst found in the spleen?
What is a felon?
According to the Parkland formula, what is the amount of Ringer's Lactate (RL) given in 24 hours for burn patients?
Leriche syndrome is caused by which of the following obstructions?
A patient with ameloblastoma of the jaw can best be treated by?
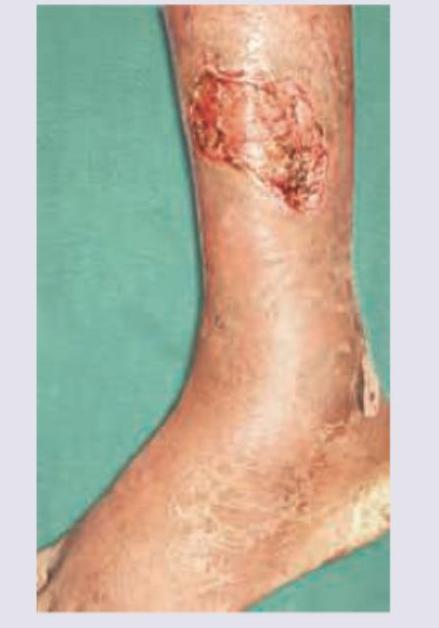
Marjolin's ulcer is a:
Which of the following has an increased risk?
Which of the following is an example of a clean-contaminated wound?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
