General Surgery Principles — MCQs

On this page
Infestation with Clonorchis sinensis increases the risk of which of the following conditions?
Alveoloplasty is performed following multiple extractions for what purpose?
A 25-year-old patient presents with a 2-cm painful abscess in the perianal region for 1 day. The patient does not have fever or leukocytosis. In which anatomical space is this lesion located?
Howship-Romberg sign is associated with which condition?
Take in of split skin graft occurs when?
Hyperbaric oxygen is indicated for which of the following conditions?
All are criteria for SIRS except?
What is the most common clinical presentation of basal cell carcinoma?
A sitz bath consists of which of the following?
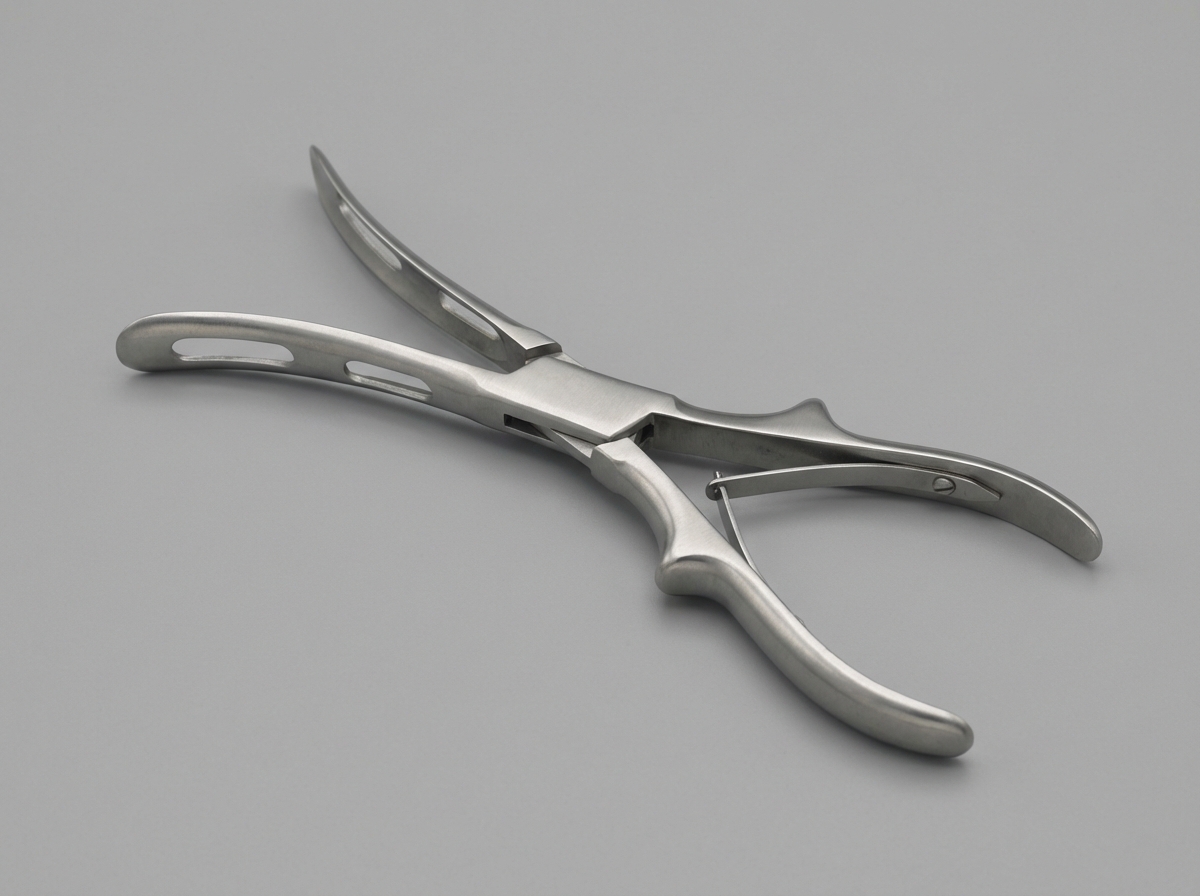
What is the instrument shown below?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
