General Surgery Principles — MCQs

On this page
All of the following are causes of pneumoperitoneum except?
Hyperacute rejection is due to which of the following mechanisms?
Bochdalek hernia occurs through which anatomical structure?
A 37-year-old woman presents with high fever (39.5°C), nausea, and vomiting. Physical examination reveals increased abdominal pain in the paraumbilical region, rebound tenderness over McBurney's point, and a positive psoas sign. Blood tests show marked leukocytosis. What is the most likely diagnosis?
Splenectomy is done to tide over the acute crises of uncontrollable:
What is true about a femoral hernia?
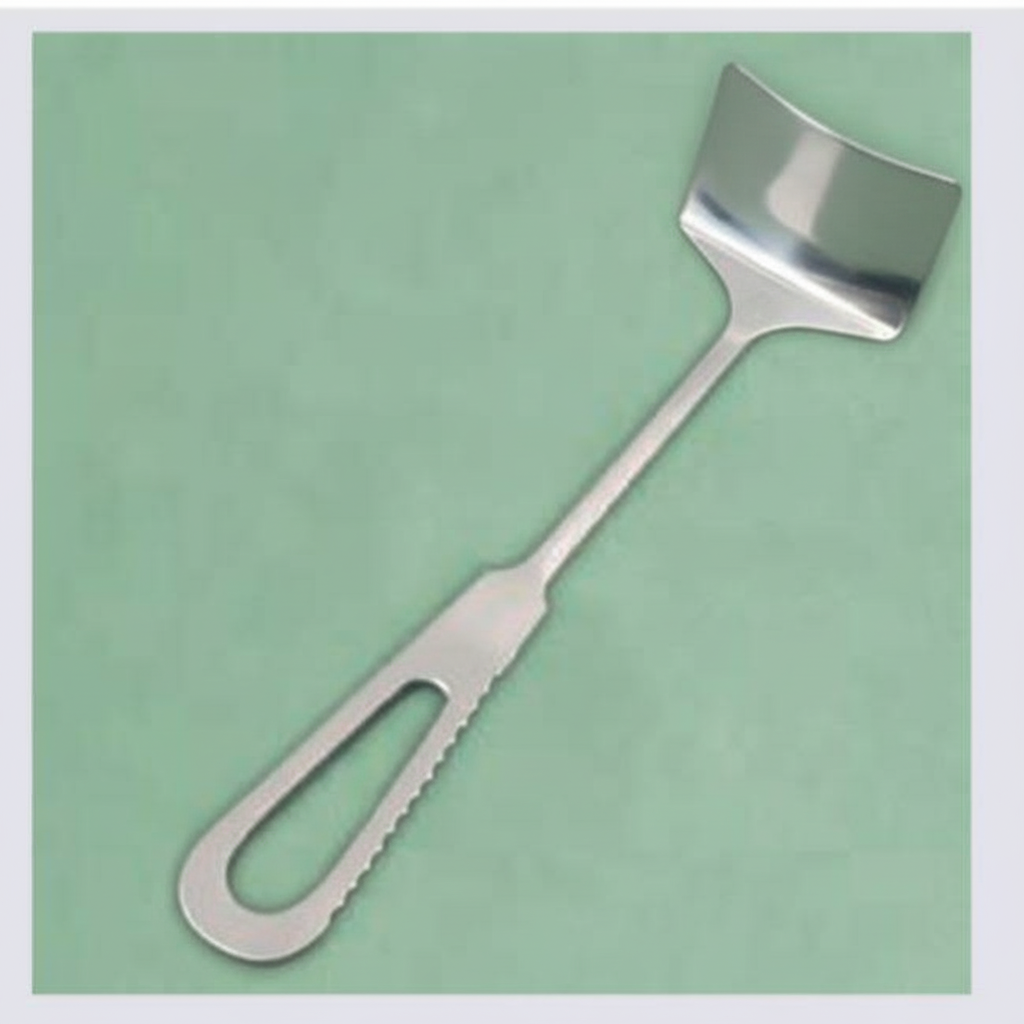
What is the name of this retractor?
A 60-year-old female presents with a tender, irreducible mass immediately below and lateral to the pubic tubercle. Plain abdominal X-ray shows intestinal obstruction. What is the most likely diagnosis?
Purulent inflammation and infection of the terminal pulp space of the distal phalanges is known as:
What is a Marjolin ulcer?
Practice by Chapter
Wound Healing and Care
Practice Questions
Surgical Infections
Practice Questions
Fluid and Electrolyte Management
Practice Questions
Nutrition in Surgical Patients
Practice Questions
Hemostasis and Blood Transfusion
Practice Questions
Surgical Instruments and Equipment
Practice Questions
Sutures and Stapling Devices
Practice Questions
Minimal Access Surgery Principles
Practice Questions
Surgical Complications
Practice Questions
Anesthesia Principles for Surgeons
Practice Questions
Surgical Oncology Principles
Practice Questions
Evidence-Based Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
