Gastrointestinal Surgery — MCQs

On this page
Paralytic ileus is caused by which of the following conditions?
What is the treatment of choice for this patient?
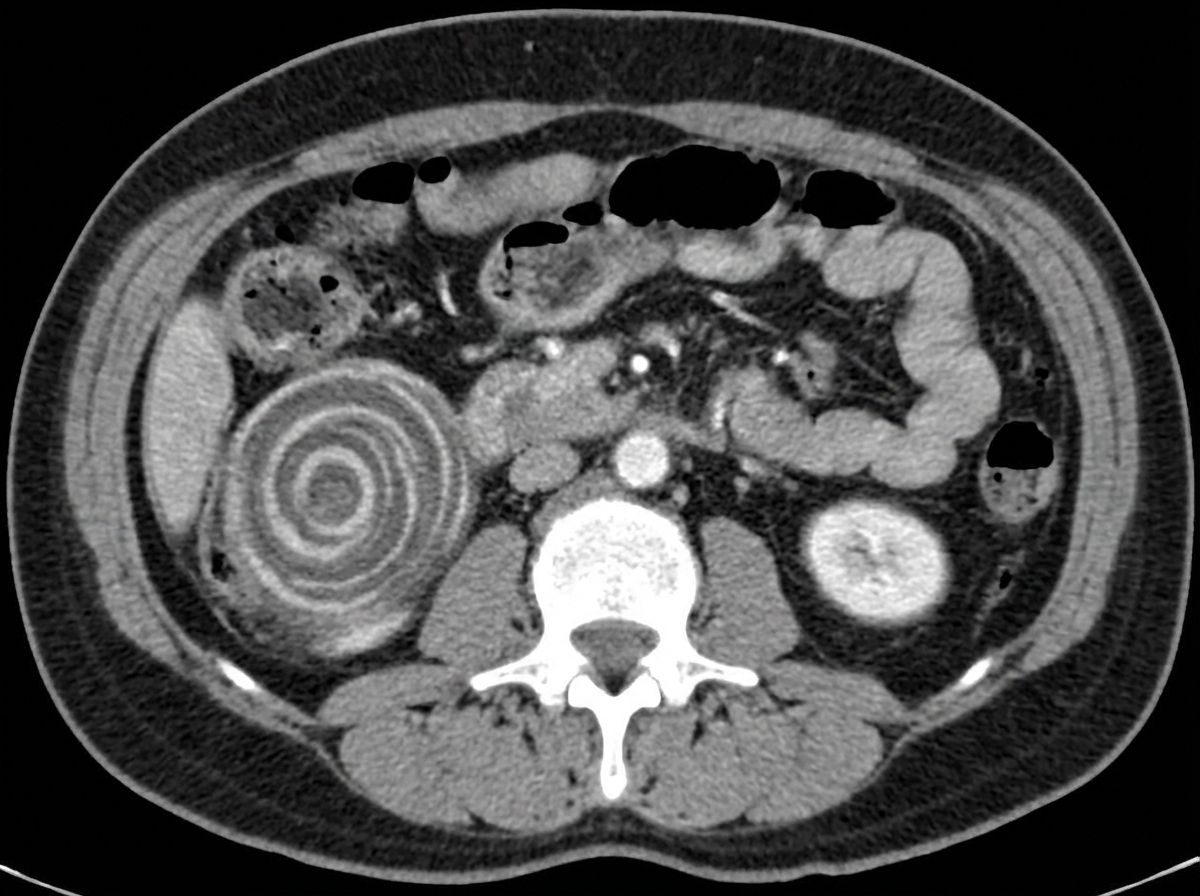
What is typically NOT seen following a massive resection of the small bowel?
Entero-enteric fistula is found in all EXCEPT:
Hourglass stomach is seen in which of the following conditions?
Post-vagotomy diarrhea can be effectively managed by which of the following?
What is the most appropriate management for advanced stage rectal carcinoma?
A posteriorly perforating ulcer in the pyloric antrum of the stomach is most likely to produce initial localized peritonitis or abscess formation in which of the following spaces?
What is the most common site of an intra-peritoneal abscess?
Which of the following is NOT true of cholelithiasis?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
