Gastrointestinal Surgery — MCQs

On this page
Malignant transformation is commonly seen in which type of ulcer?
All are true about acute appendicitis except:
Which is the most common site for iatrogenic esophageal perforation?
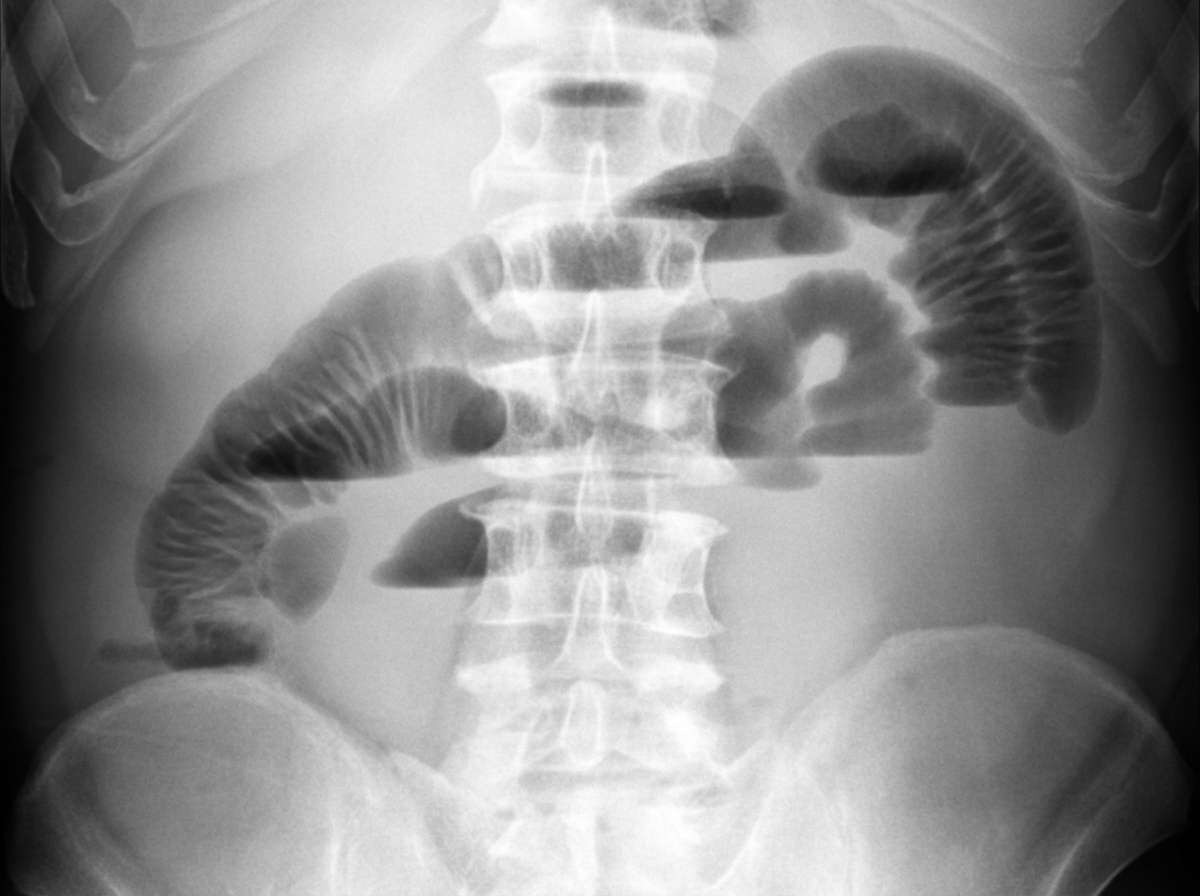
A 24-year-old man presents to the emergency department with a 12-hour history of intermittent, crampy abdominal pain and five episodes of vomiting. He denies any rectal bleeding. On examination, his abdomen is distended with absent bowel sounds. Per-rectal examination is normal. An abdominal X-ray reveals findings suggestive of a specific condition. Based on the X-ray findings, which of the following statements are true?
Highest incidence of acute appendicitis occurs in which decade of life?
What is the most common cause of upper gastrointestinal bleeding?
Which investigations are needed in intestinal obstruction?
What is the treatment of choice for a bleeding gastric ulcer?
A 64-year-old male presented with severe diarrhea, having more than 20 bowel movements per day, following an elective operation for duodenal ulcer disease. Medications have been ineffective. The exact details of his operation cannot be ascertained. What operation was most likely performed?
What is the indication for PAIR treatment in a hydatid cyst?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
