Gastrointestinal Surgery — MCQs

On this page
What is the investigation of choice in diffuse esophageal spasm?
Which of the following statements is NOT true regarding gastrointestinal tuberculosis?
Which of the following statements is true about appendicular rupture?
Which is the most common cause of the below condition?
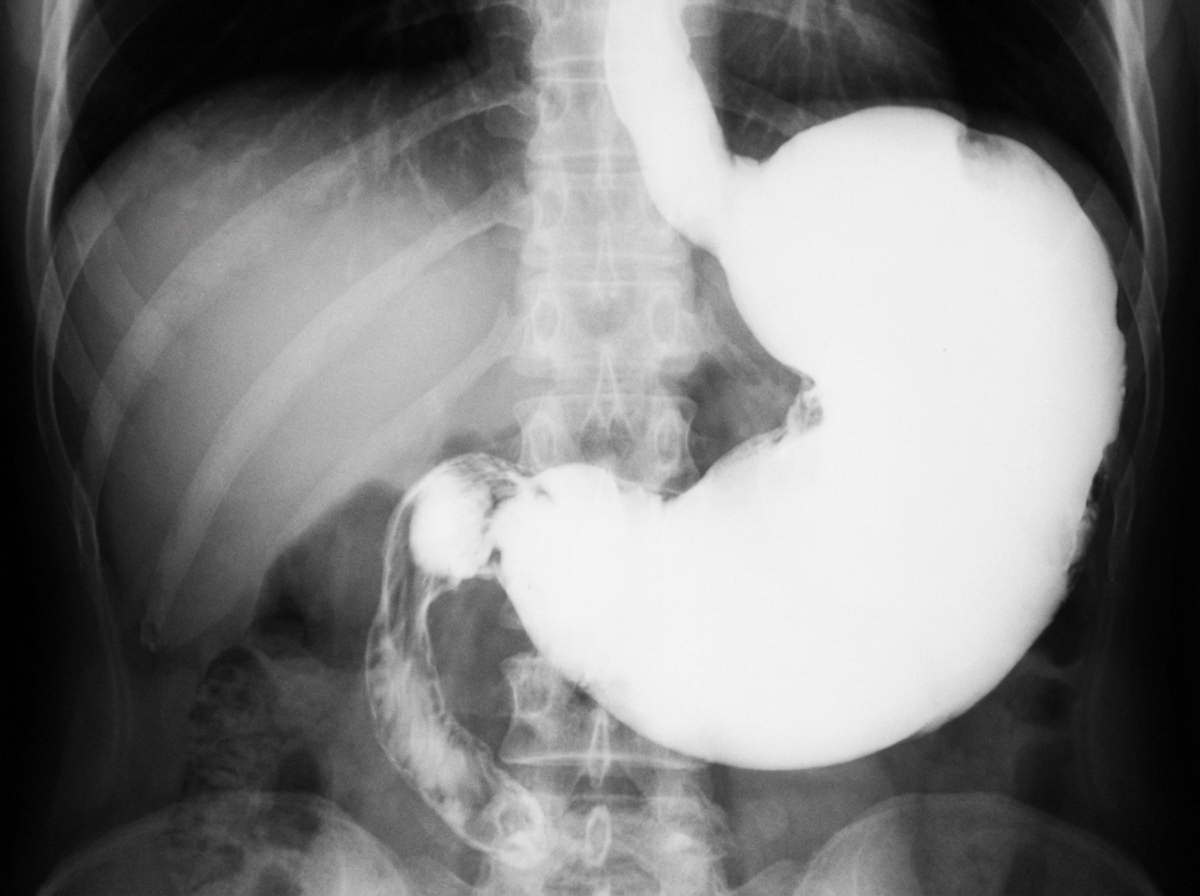
A patient with a gastric ulcer has a biopsy that reveals malignancy. What is the next step in management?
Regarding Achalasia Cardia, which of the following statements are true?
What is the common site of regional enteritis?
All of the following are indications for surgery in a case of duodenal ulcer except?
Which of the following statements about carcinoid of the appendix is NOT TRUE?
An elderly patient presents with a prolonged history of weakness and lethargy. On examination, he is found to be anemic and stool is positive for occult blood. Which of the following is the investigation of choice?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
