Gastrointestinal Surgery — MCQs

On this page
A patient presents with non-progressive dysphagia exclusively for solids. A barium study reveals proximal esophageal dilatation with distal constriction. What is the most likely diagnosis?
What is the most important cause of abdominal distension in intestinal obstruction?
Which of the following is NOT a risk factor for post-ERCP pancreatitis?
Which of the following is not a surgical treatment for GERD?
What are the similarities between fissure in ano and achalasia cardiae?
Which of the following is considered a true diverticulum?
What is the most common cause of generalized peritonitis in a 40-year-old adult male?
A female patient complains of periumbilical pain and nausea, particularly after taking food. What is the most likely diagnosis?
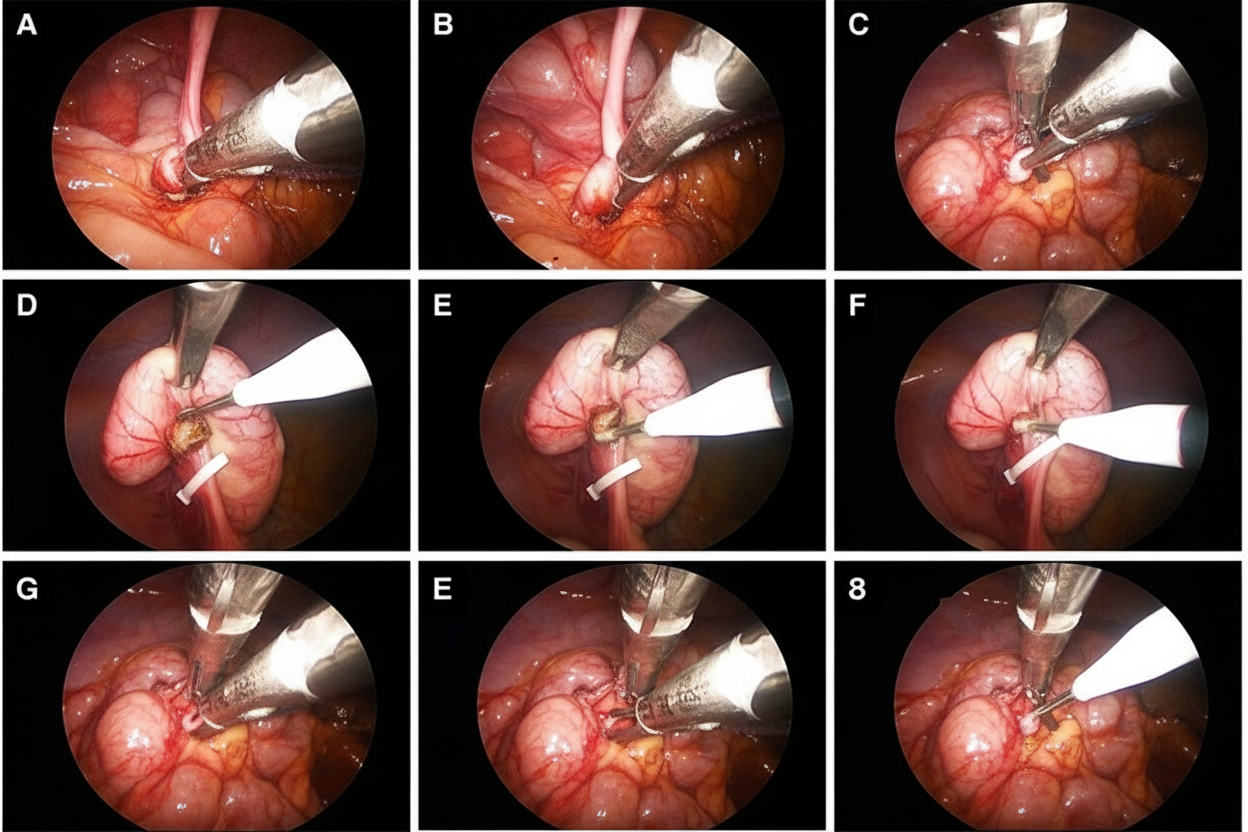
What scoring system is used to diagnose the condition for which the surgery below was performed?
Which of the following is NOT a characteristic of esophageal cancer?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
