Gastrointestinal Surgery — MCQs

On this page
Which of the following statements is not true about Schatzki's ring?
What is the most common tumor of the small intestine?
What is the most common presentation of carcinoma of the right colon?
Which of the following staging systems is used for gastroesophageal reflux disease (GERD)?
During an operation for presumed appendicitis, the patient's appendix is found to be markedly thickened and feels rubbery to firm. The serosa is edematous and inflamed, and the mesentery is thickened with fat growing about the bowel circumference. What is the most likely diagnosis?
Diffuse peritonitis following appendicitis is usually seen when?
Peptic ulcers located in which site are most likely to perforate?
Which of the following is the most common complication of appendectomy?
The below instrument is used for the treatment of:
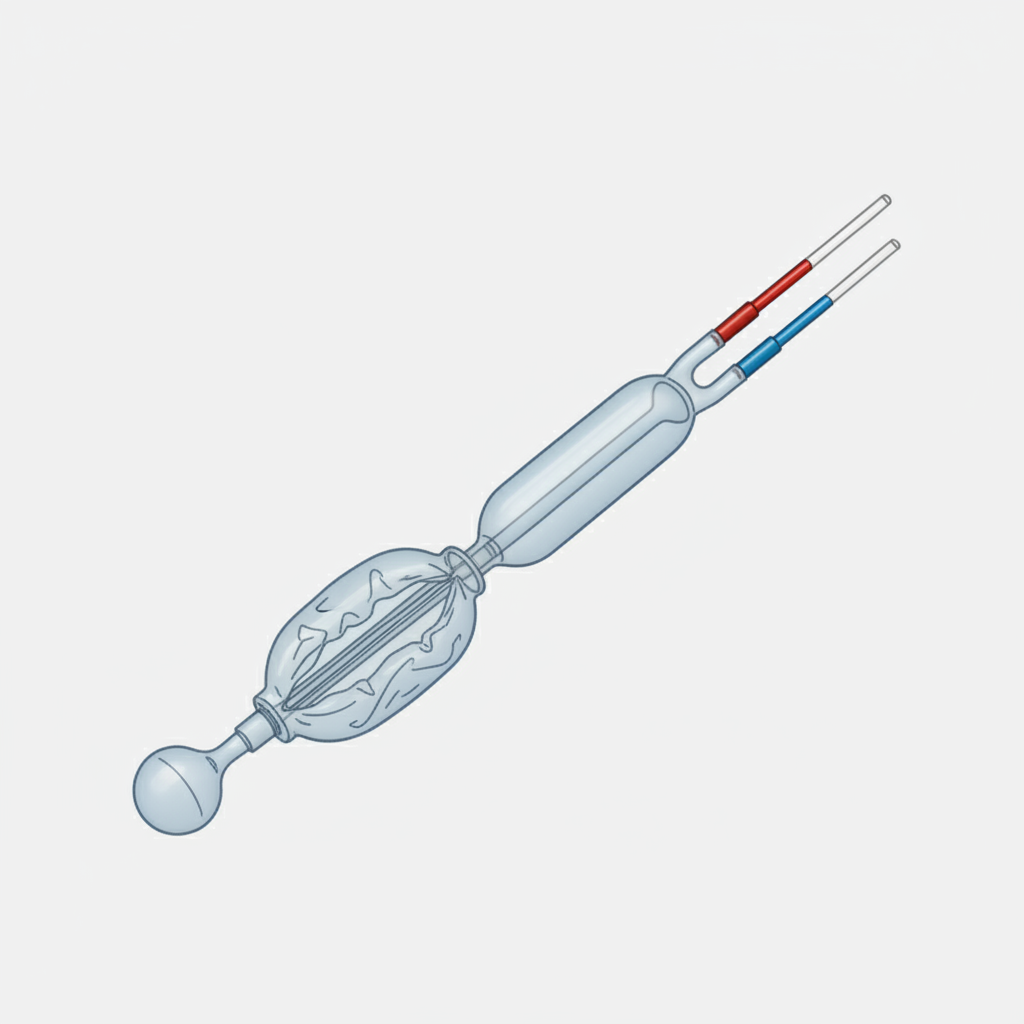
Which artery is most commonly responsible for bleeding in duodenal ulcer hemorrhage?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
