Gastrointestinal Surgery — MCQs

On this page
What is a 'duodenal blowout'?
What is true about a patient with a right subphrenic abscess?
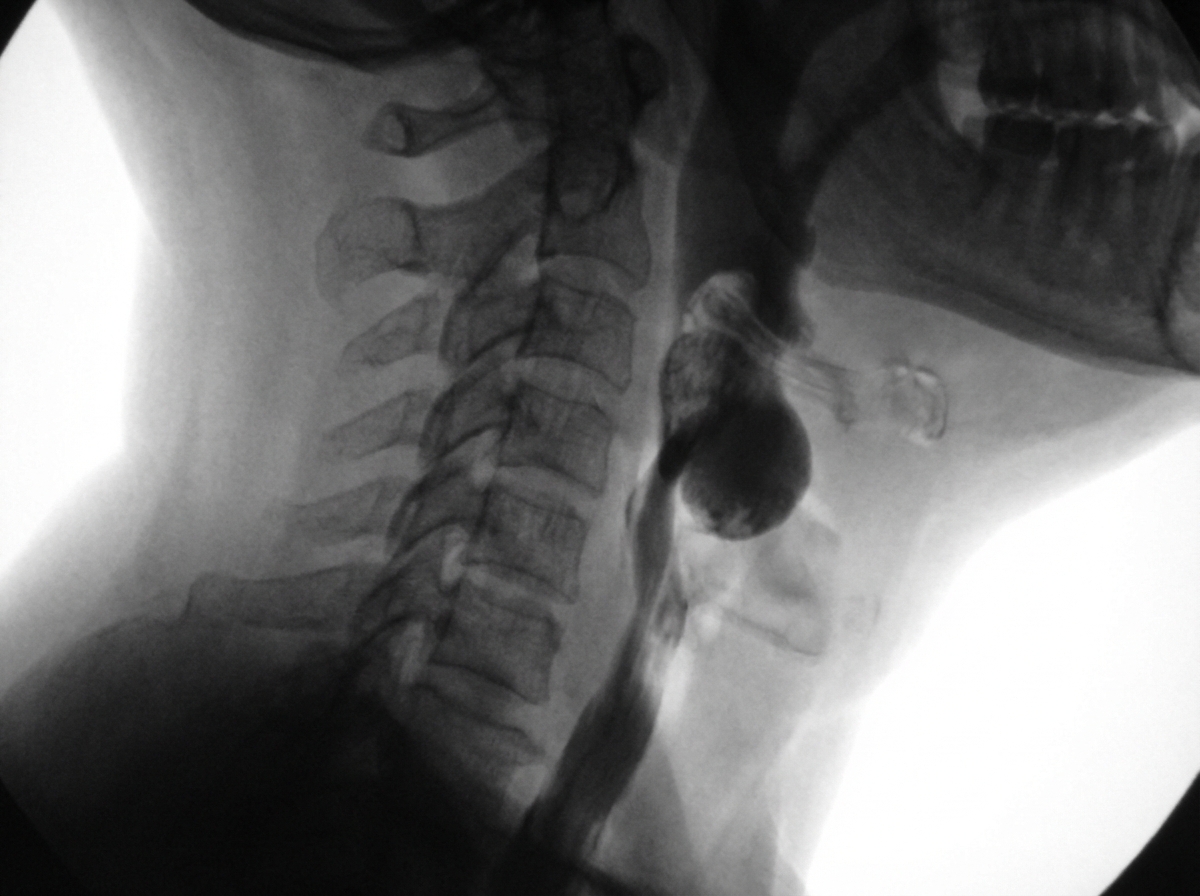
A 74-year-old male complains of bad breath, regurgitation of food during his sleep, and weight loss. For several months he has also had trouble swallowing solids. He denies fever, chills, and nausea. The patient does not smoke cigarettes and does not drink alcohol. Barium swallow study with fluoroscopy is obtained. Which of the following is the most likely underlying cause of the patient's condition?
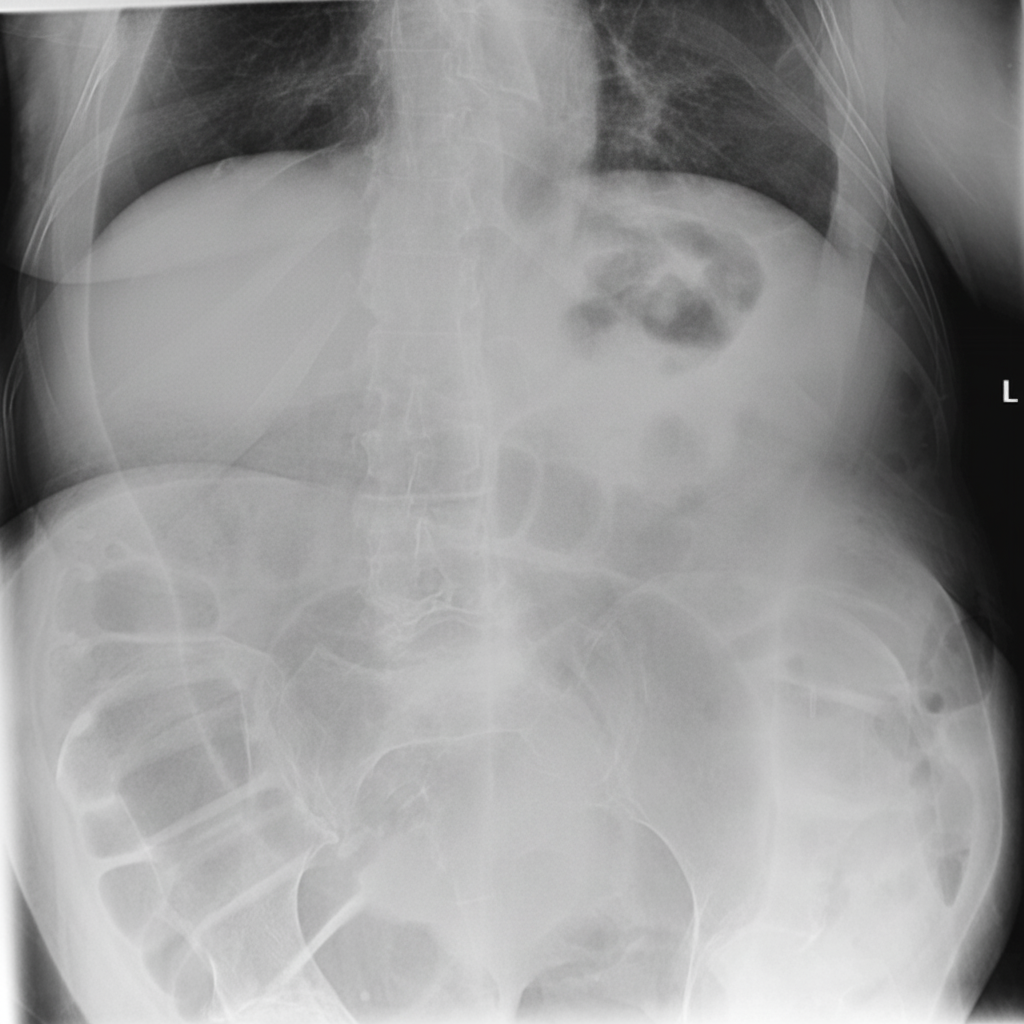
Multiple strictures in the intestine are found in which condition?
What condition is characterized by increasing difficulty in swallowing both solids and liquids, along with a bird's beak appearance on X-ray?
Which among the following is the commonest site of diverticulosis in the old population?
An elderly male presents with gradually increasing dysphagia more for solids, hoarseness of voice, and a palpable cervical node. What is the most likely diagnosis?
The lowest recurrence of peptic ulcer is associated with which surgical procedure?
All of the following are true about carcinoid crisis, EXCEPT:
What is the etiology for this condition?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
