Gastrointestinal Surgery — MCQs

On this page
A 58-year-old lady is diagnosed with carcinoma of the stomach. A CT scan of the abdomen shows a 4 cm mass in the antrum with involvement of the serosa. What is the treatment?
All the following polyps are premalignant except:
A female patient presents with dysphagia and intermittent epigastric pain. Endoscopy reveals esophageal dilatation above and narrowing at the lower end. What is the recommended treatment?
Mortality rate is higher among which of the following conditions?
Snow storm ascites is seen in which of the following conditions?
Which of the following investigations is useful in the evaluation of upper gastrointestinal bleeding?
Boerhaave syndrome is the spontaneous rupture of which part of the esophagus?
A 23-year-old lady presents with acute right lower abdominal pain for the past 4 hours. There is tenderness at McBurney's point. Which investigation is best suited to confirm the diagnosis of appendicitis?
What is the best investigation to diagnose colonic diverticulosis?
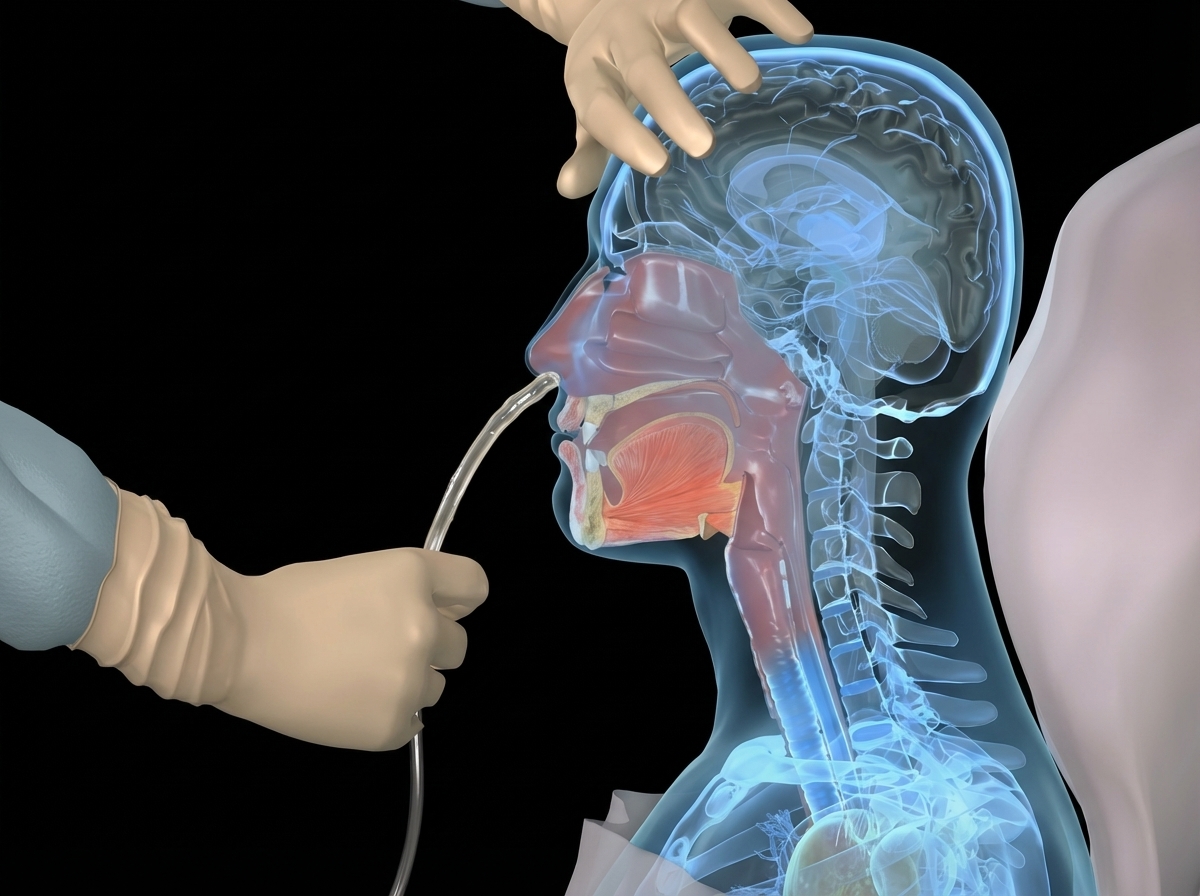
Which of the following is the primary use of the nasogastric tube depicted?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
