Gastrointestinal Surgery — MCQs

On this page
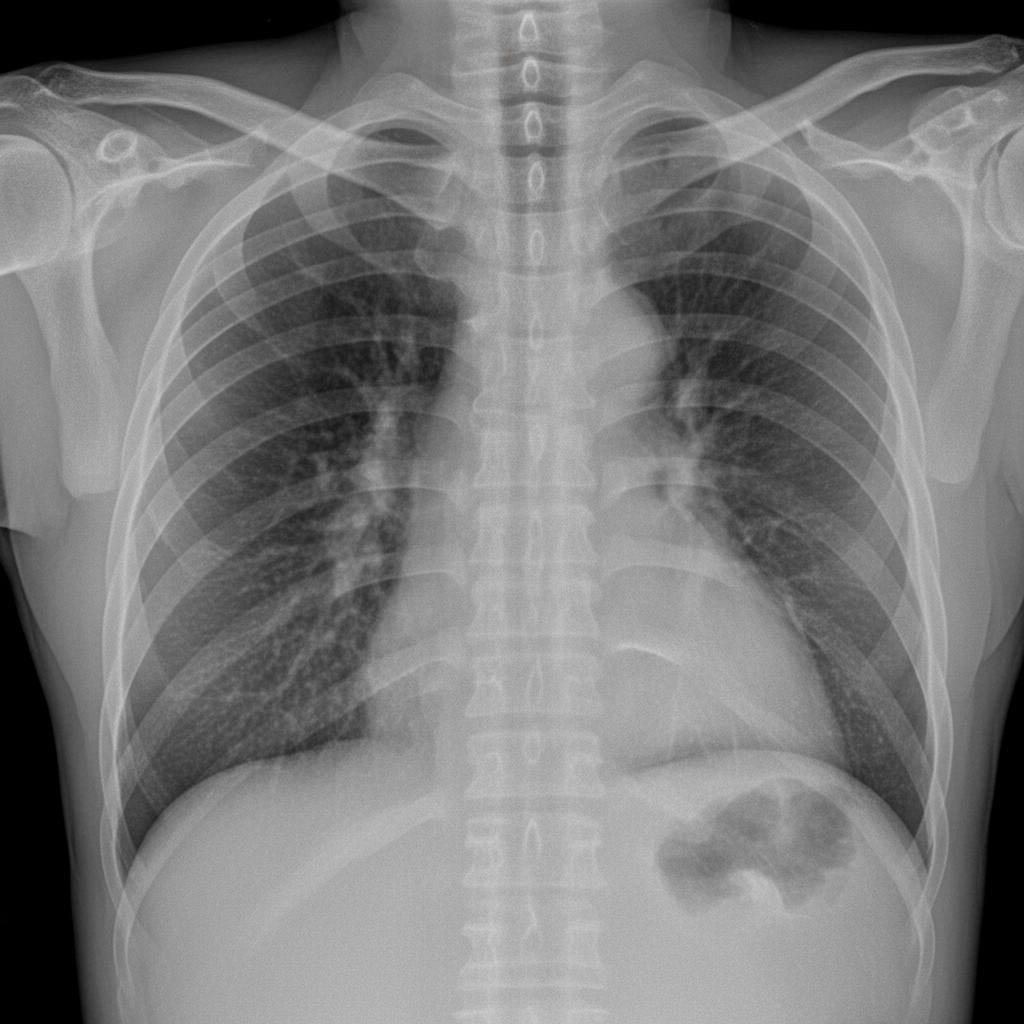
A 45-year-old male with a history of chronic duodenal ulcer presented to the emergency department in a state of shock. After resuscitation, investigations were performed. A chest X-ray is provided. What is the preferred treatment option?
Which of the following is false regarding Barrett's esophagus?
Which of the following treatment modalities is NOT used for the management of acute blood loss due to ruptured esophageal varices?
Indications for surgery in Bronchiectasis include all of the following except?
Which of the following is a predisposing factor for carcinoma of the esophagus?
Cattle's maneuver is mobilization of:
Which of the following statements about Zenker's diverticulum is TRUE?
A 50-year-old male presented with progressive dysphagia for 4 months to solids, significant weight loss, loss of appetite, odynophagia, a hoarse voice, and cervical lymphadenopathy. Upper GI endoscopy with biopsy was performed. Which of the following barium findings would most likely correspond with this condition?
In intestinal anastomosis, what layer primarily provides strength?
Which of the following statements is NOT true regarding Curling's ulcer?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
