Gastrointestinal Surgery — MCQs

On this page
What is true about Peutz-Jeghers syndrome?
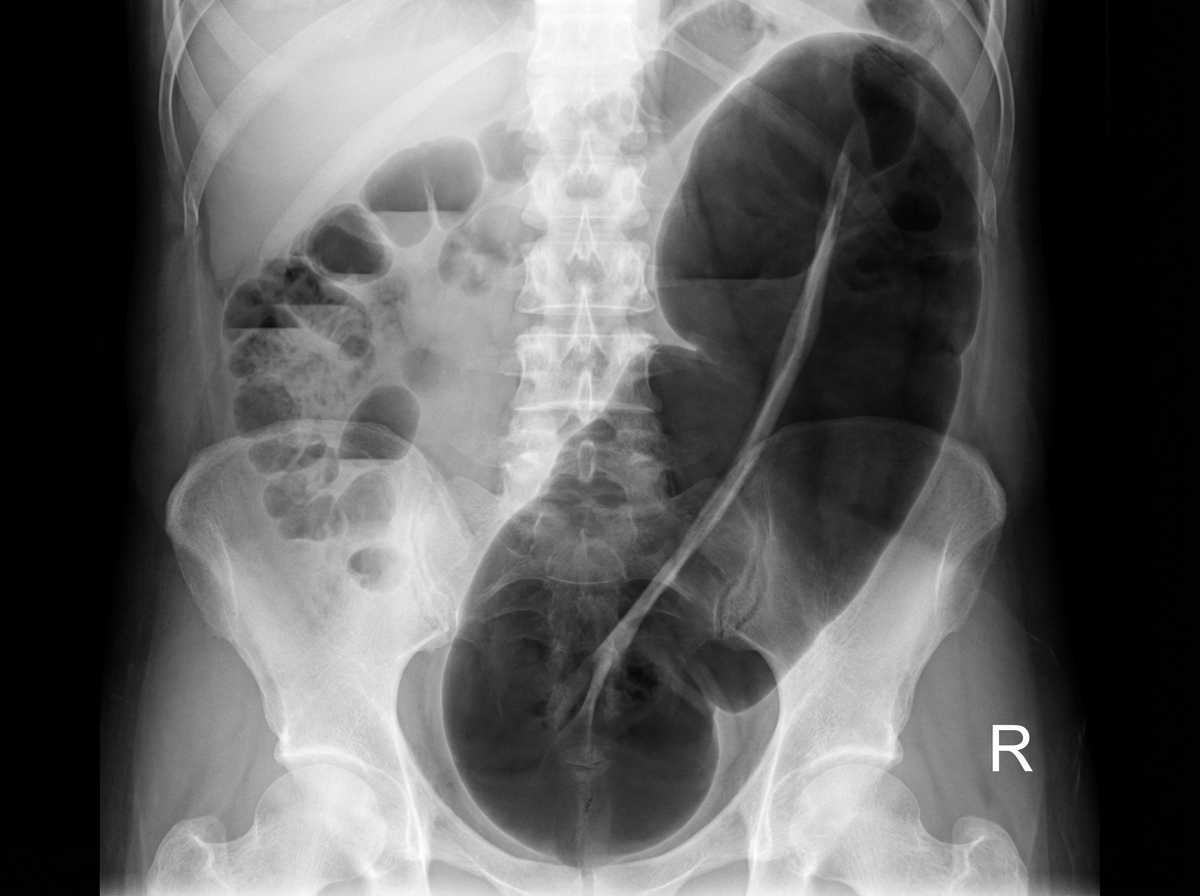
An X-ray of the abdomen reveals a specific finding. Identify the finding and its associated pathology:
Which of the following is NOT true about appendicular rupture?
What permanent deleterious effects are seen if 25% of the small intestine is resected?
Hiatus hernia is treated by:
What is the earliest manifestation observed after a gastrectomy?
Which of the following statements is false regarding the Sengstaken-Blakemore tube?
Which of the following is NOT true about hyperplastic tuberculosis?
What is the most common complication of achalasia?
High-resolution manometry is the investigation of choice in all except:
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
