Gastrointestinal Surgery — MCQs

On this page
What is the aim of preventing reflux esophagitis by repairing a hiatus hernia?
In a highly selective vagotomy, the vagal supply is severed to which part of the stomach?
Which of the following colonic polyps has the highest potential for malignant transformation?
What is the commonest site from which pseudomyxoma peritonei arise?
Regarding typhoid ulcer, all of the following are true except?
What is the standard treatment of an appendicular mass?
What is the most common site of carcinoma of the esophagus?
Who performed the first gastrectomy in 1881?
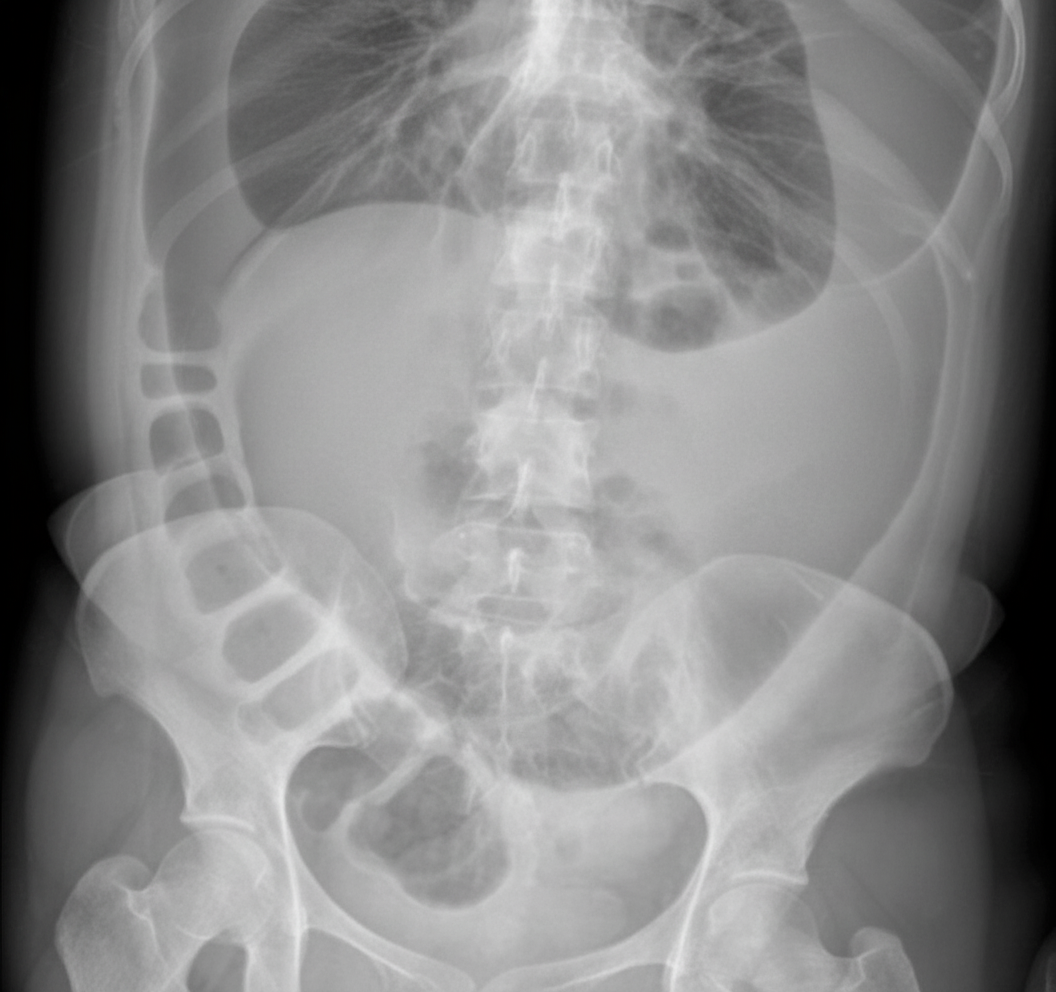
A 70-year-old male presents with colicky pain in the lower abdomen, with non-passage of feces and flatus. Abdominal X-ray findings are provided. Which of the following is the preferred treatment option for this patient?
What is the most common cause of free air under the diaphragm?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
