Gastrointestinal Surgery — MCQs

On this page
Primary peritonitis is more common in females because:
In Duke's classification of cancer rectum, what does stage B2 denote?
A 63-year-old man undergoes a partial gastrectomy with Billroth II reconstruction for intractable peptic ulcer disease. He presents several months postoperatively with a megaloblastic anemia. Which of the following is the best treatment for this surgical complication?
Malignant transformation is commonly seen in which of the following conditions?
Which condition is diagnosed by the following sign?
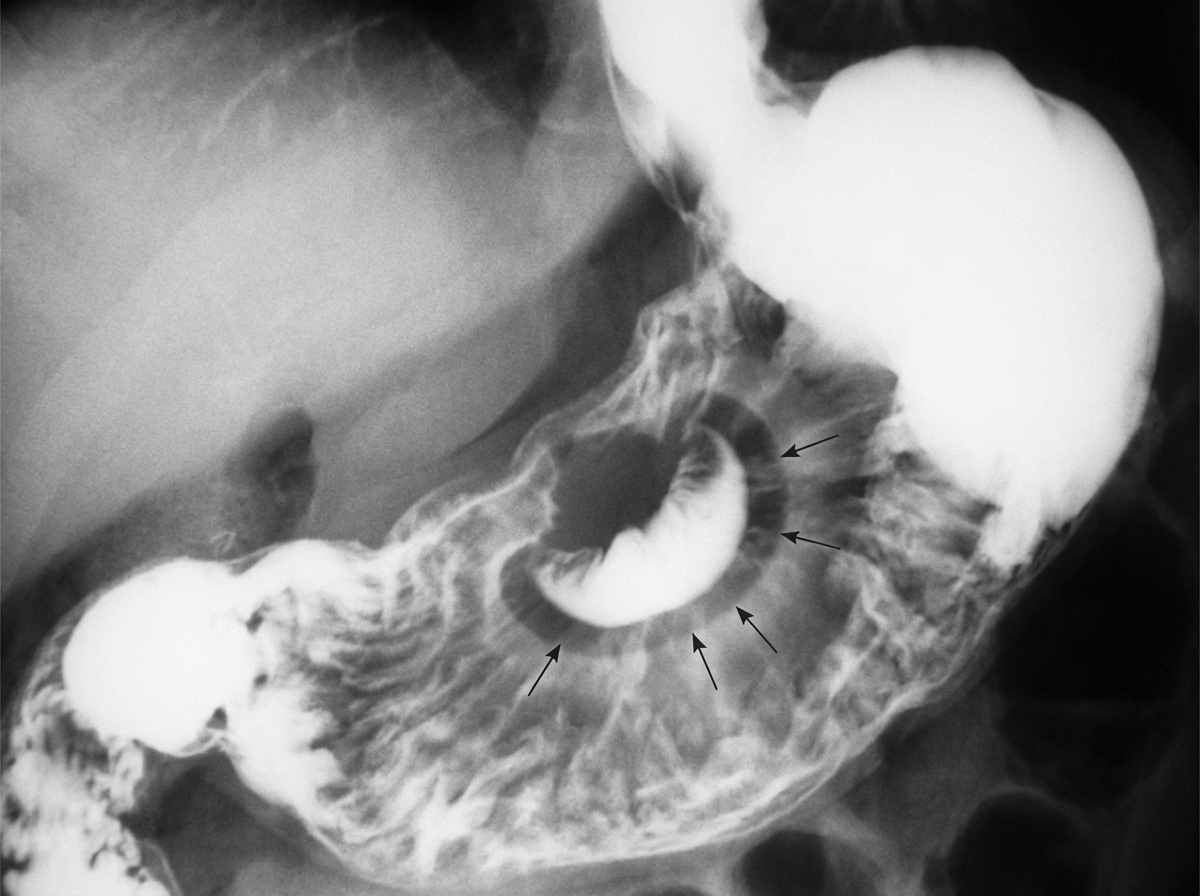
Reflux esophagitis is common in which type of hiatus hernia?
A 24-year-old man presents with symptoms of acute intestinal obstruction. His temperature is 38°C (101°F), respirations are 25 per minute, and blood pressure is 120/80 mm Hg. Physical examination reveals a mass in the right lower abdominal quadrant. Laparoscopy shows numerous small bowel strictures and a fistula extending into a loop of small bowel. Which of the following is the most likely diagnosis?
Which of the following is false regarding cecal volvulus?
Which condition presents with a 'bird's beak' appearance?
Lung volume reduction surgery is used in the management of which of the following conditions?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
