Gastrointestinal Surgery — MCQs

On this page
What is the investigation of choice to determine the depth of cancer invasion?
Which of the following can be used in the management of acute pancreatitis?
A 21-year-old patient attended a party the previous night and presents with the following symptoms: pain in the abdomen radiating to the back, pulse of 100/min, BP of 100/76 mmHg, temperature of 39°C, and vomiting. What is the most probable diagnosis?
What is a trichobezoar?
All of the following statements about Zenker's diverticulum are true, except?
Which of the following conditions does NOT typically present with bleeding per rectum?
A patient complains of epigastric pain radiating to the back. What is the investigation of choice?
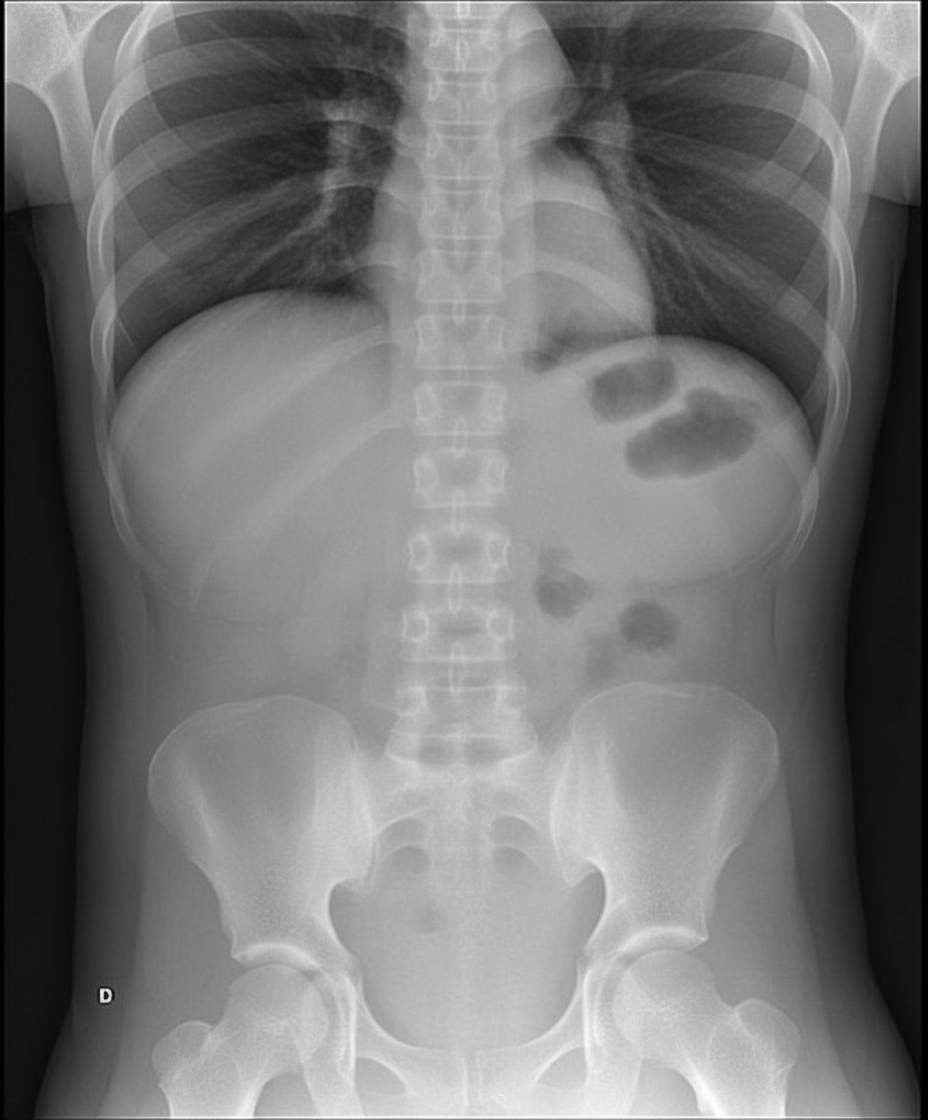
A patient presents with abdominal distention, nausea, and vomiting, reporting a long history of intermittent obstructive symptoms and distention. Radiological examination shows the following presentation. Which of the following statements regarding the treatment of this condition is false?
Which of the following statements about gastric carcinoma is incorrect?
What is the most common nutritional deficiency observed after a gastrectomy?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
