Gastrointestinal Surgery — MCQs

On this page
Most common site of chronic gastric ulcer:
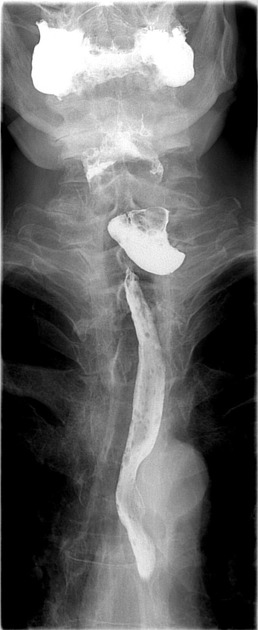
A 70 year old patient presented with history of fever, repeated aspiration and coughing in the night. On examination there is a swelling on left side of neck which produces gurgling sound on compression. Following is the barium swallow study of the patient. What is the most likely diagnosis?
A patient presents with abdominal pain, blood in stools and a palpable mass on examination. A Barium Study was performed, probable diagnosis is?
Which layer differentiates Boerhaave syndrome from Mallory-Weiss tear in terms of depth of involvement?
True about Mallory-Weiss tear is:
A 40-year-old male with right iliac fossa pain, fever. CT shows 4cm appendix with faecolith. Best management?
A 25-year-old patient presents with RLQ pain, fever, and vomiting. CT shows a ruptured appendix. What is the next step?
Which of the following findings on physical exam suggests a strangulated inguinal hernia?
What is the typical presentation of acute appendicitis?
What is the definitive treatment for gallstone-induced pancreatitis?
Practice by Chapter
Esophageal Disorders
Practice Questions
Gastric Disorders
Practice Questions
Small Intestine Pathology
Practice Questions
Appendicitis
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Diverticular Disease
Practice Questions
Anorectal Disorders
Practice Questions
Colorectal Neoplasms
Practice Questions
Gastrointestinal Stomas
Practice Questions
Bariatric Surgery Principles
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
