Diverticular Disease — MCQs

Which of the following is NOT characteristic of lymphogranuloma venereum proctitis?
Emergency management of Ulcerative colitis is by:
The most common complication of Zenker's diverticulum is:
What is the treatment of choice for a 70-year-old male patient who presents with peritonitis secondary to ruptured diverticulitis?
Which of the following conditions is not reduced by a high-fiber diet?
A patient presents with abdominal pain, blood in stools and a palpable mass on examination. A Barium Study was performed, probable diagnosis is?
Massive bleeding per rectum in an elderly patient is due to.
Dohlman surgery in Zenker's diverticulum is:-
A 40-year-old male with gastroesophageal reflux disease (GERD) is found to have Barrett's esophagus with low-grade dysplasia on endoscopy. What is the most appropriate initial pharmacological treatment for this condition?
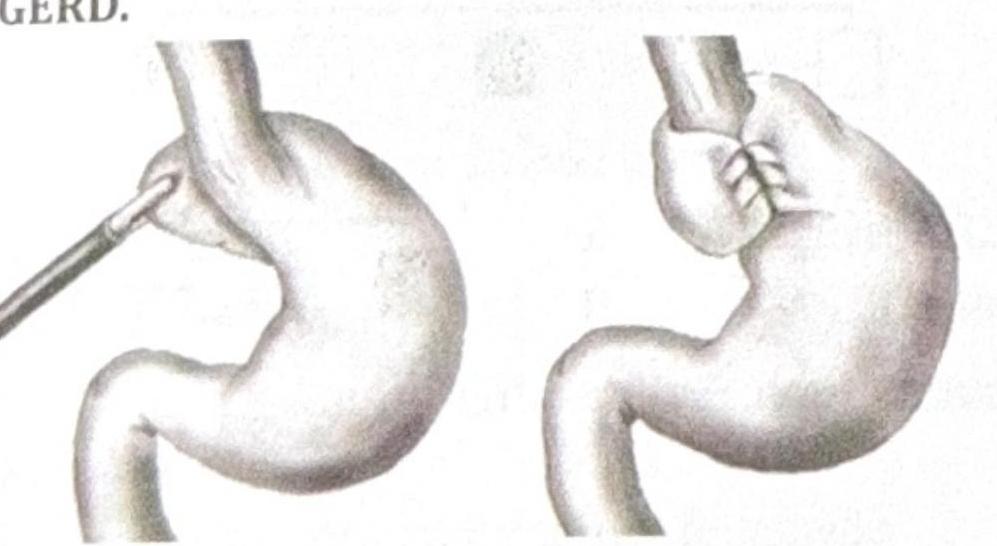
Identify the procedure shown in the image, which is performed in a patient with recurrent GERD.
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
