Endocrine Surgery — MCQs

On this page
What is the standard incision used in thyroidectomy?
The specimen shown below is:
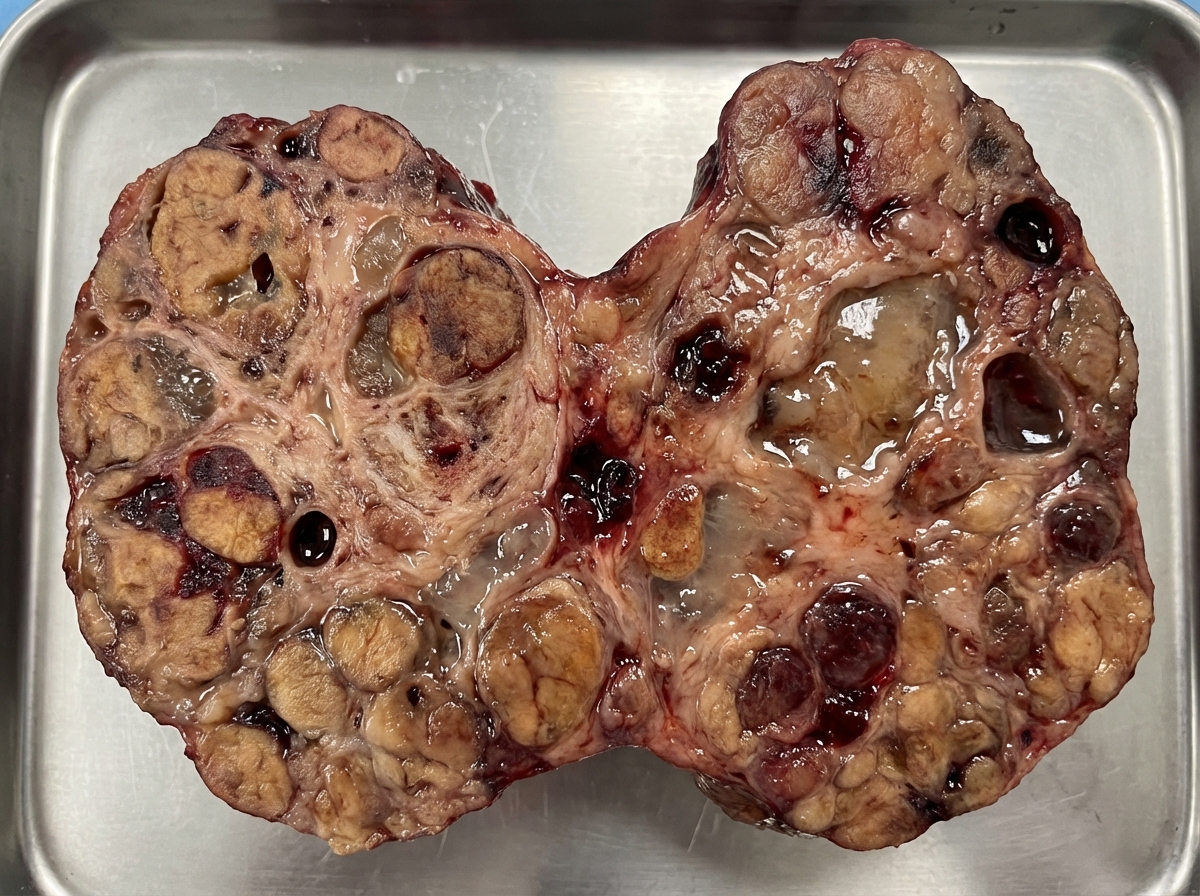
What is tense and painful thyroiditis?
Which of the following carcinomas shows a good response to radioiodine?
A middle-aged female presents to the surgical OPD with a thyroid swelling. She has a history of Hodgkin's lymphoma. Which of the following thyroid malignancies is most likely to be suspected in this patient?
Which of the following statements regarding follicular cell carcinoma of the thyroid is true?
What is the recommended treatment for papillary carcinoma of the thyroid with lymph node metastasis at level VI?
What is the treatment for a brown tumor?
During bilateral adrenalectomy, what is the appropriate timing for the intra-operative dose of hydrocortisone?
All are true about the effect of thymectomy, EXCEPT:
Practice by Chapter
Thyroid Nodules
Practice Questions
Thyroid Cancer
Practice Questions
Graves' Disease
Practice Questions
Thyroiditis
Practice Questions
Primary Hyperparathyroidism
Practice Questions
Secondary and Tertiary Hyperparathyroidism
Practice Questions
Adrenal Cortical Tumors
Practice Questions
Pheochromocytoma
Practice Questions
Adrenal Incidentalomas
Practice Questions
Multiple Endocrine Neoplasia
Practice Questions
Neuroendocrine Tumors
Practice Questions
Intraoperative Monitoring in Endocrine Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
