Colorectal Surgery — MCQs

On this page
A patient with an abdominal wall desmoid tumor should also be screened for which of the following?
What is the best surgical procedure for mid rectal carcinoma?
All are true regarding rectal carcinoma EXCEPT?
What is the most common presentation of carcinoma of the rectum?
Prophylactic polypectomy is indicated in which of the following conditions?
Which of the following is NOT a cause of acute anal pain?
What is the recommended treatment for squamous cell carcinoma of the anal canal in a 46-year-old healthy man who does not require a colostomy?
Which statement is false regarding familial adenomatous polyposis?
All of the following are common features of hemorrhoids except?
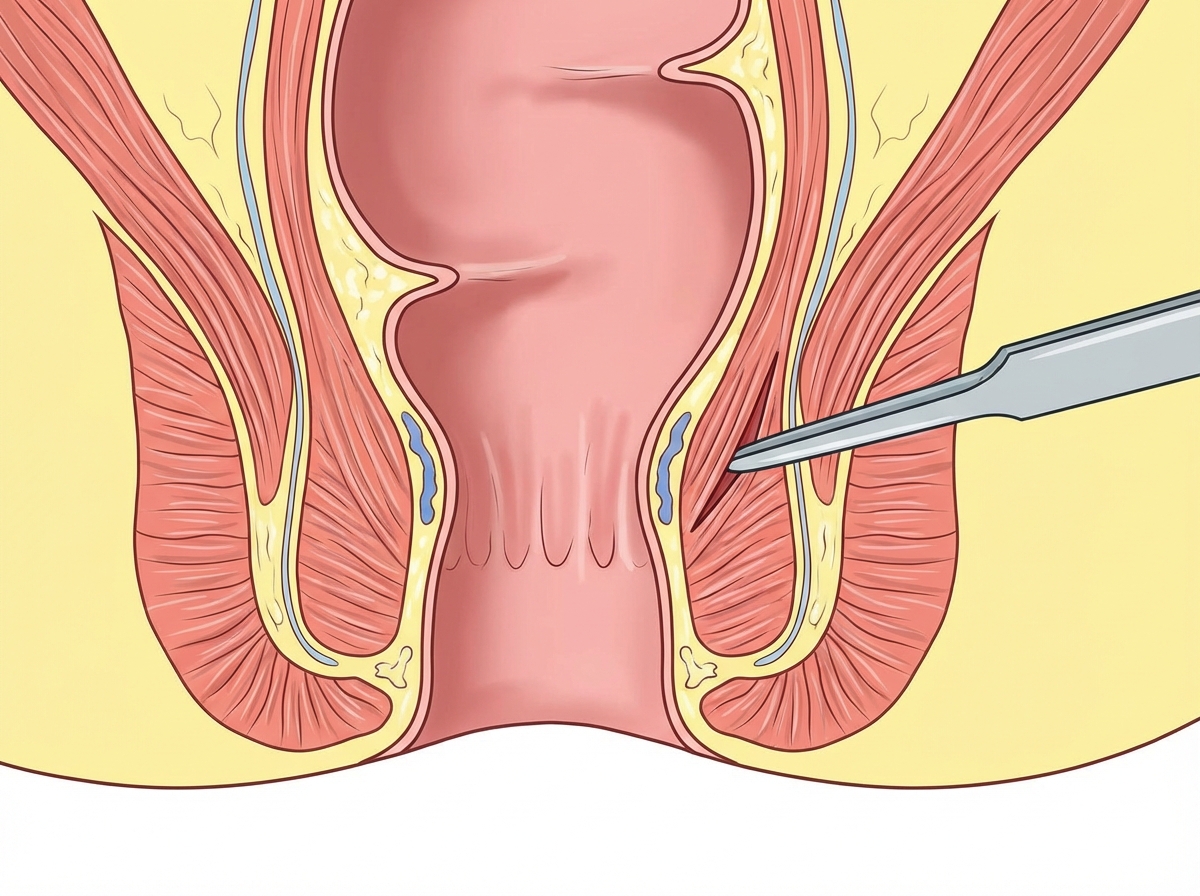
What is the condition for which the treatment shown below is followed?
Practice by Chapter
Colorectal Anatomy and Physiology
Practice Questions
Diverticular Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Colorectal Polyps
Practice Questions
Colorectal Cancer
Practice Questions
Anorectal Abscess and Fistula
Practice Questions
Hemorrhoids
Practice Questions
Rectal Prolapse
Practice Questions
Fecal Incontinence
Practice Questions
Intestinal Stomas Creation and Management
Practice Questions
Pelvic Floor Disorders
Practice Questions
Enhanced Recovery After Colorectal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
