Colorectal Surgery — MCQs

On this page
What surgery is shown here in the image?
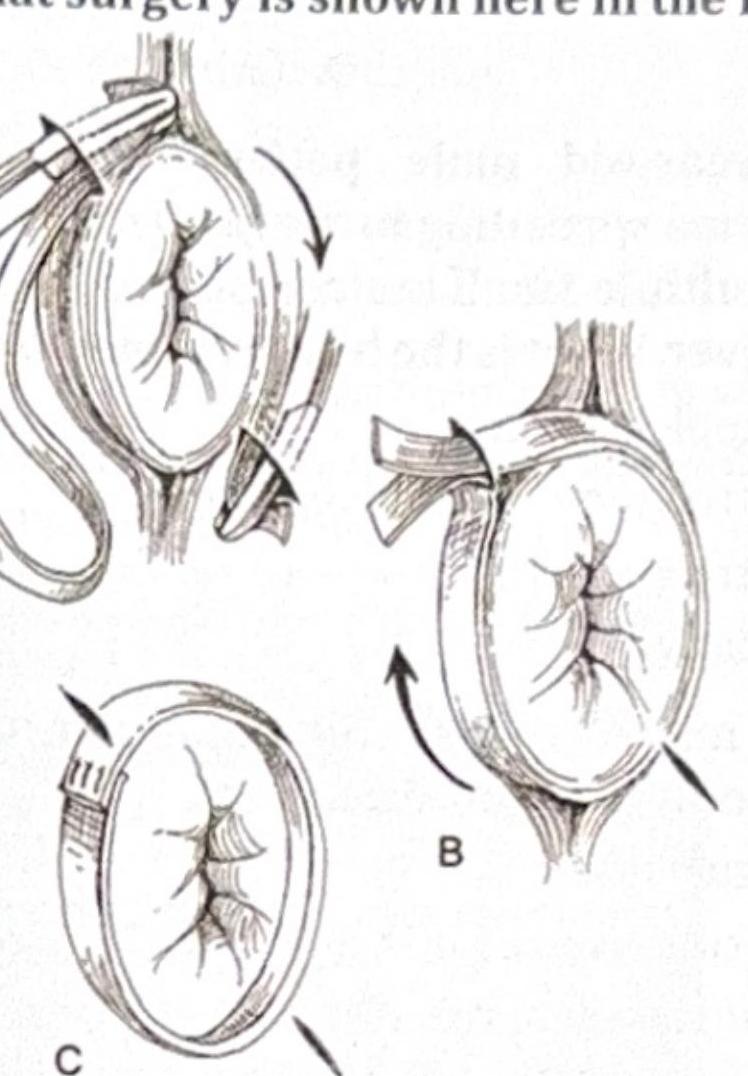
Which of the following is not a perineal approach for the condition shown in the image?
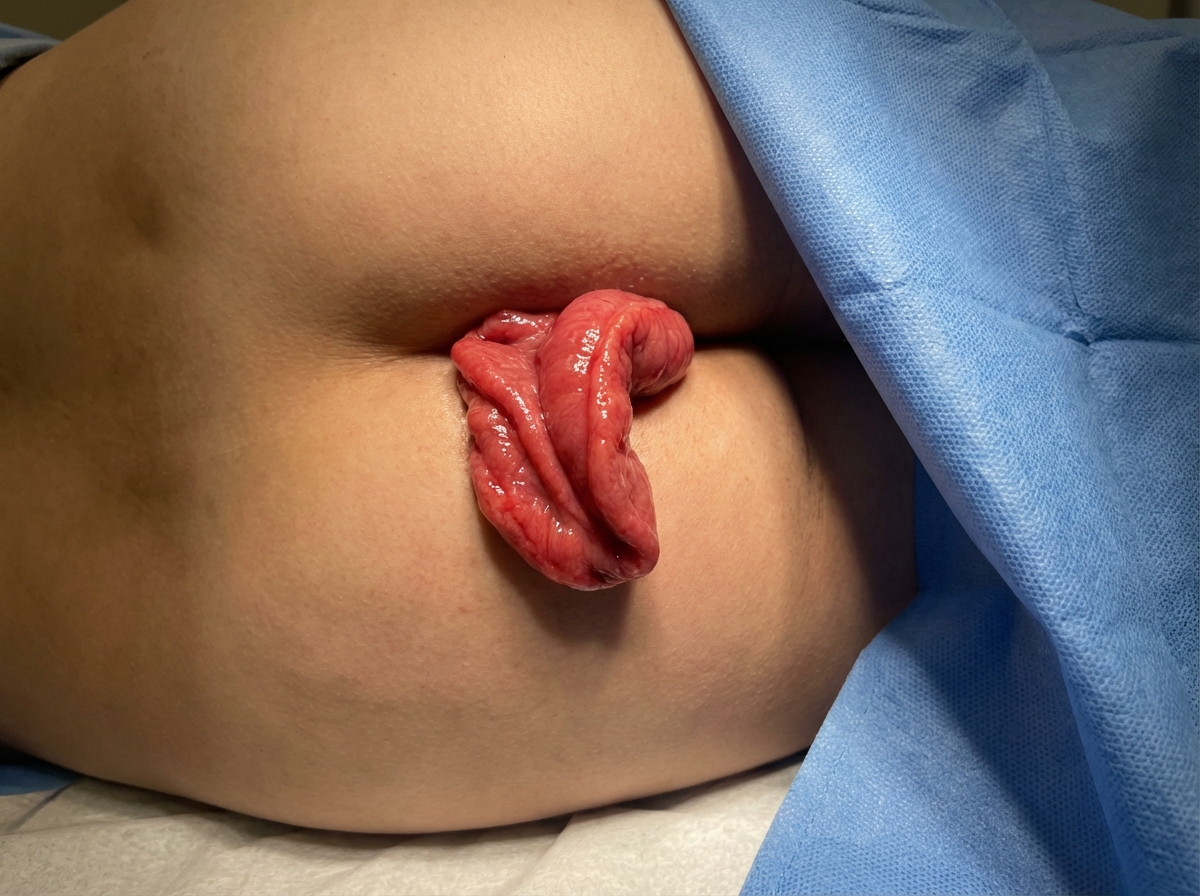
A 53-year-old patient presents with per rectal bleeding. Which is the most appropriate investigation to evaluate for colorectal pathology?
A patient with a complex rectovaginal fistula (secondary to obstetric trauma with tissue loss) should be initially treated with
Which is the most common site for colorectal cancer metastasis?
What is the most common symptom of rectal prolapse?
A 60-year-old male presents with rectal bleeding and a palpable mass on digital rectal examination. A biopsy confirms adenocarcinoma. What is the best initial step in management?
Which surgical procedure is commonly used to treat severe ulcerative colitis?
A 70-year-old male presents with a long history of constipation and straining during defecation. He reports a sensation of a bulge from the rectum. What is the most appropriate surgical treatment?
What is the most appropriate management for a patient with confirmed diverticulitis and an abscess larger than 4 cm?
Practice by Chapter
Colorectal Anatomy and Physiology
Practice Questions
Diverticular Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Colorectal Polyps
Practice Questions
Colorectal Cancer
Practice Questions
Anorectal Abscess and Fistula
Practice Questions
Hemorrhoids
Practice Questions
Rectal Prolapse
Practice Questions
Fecal Incontinence
Practice Questions
Intestinal Stomas Creation and Management
Practice Questions
Pelvic Floor Disorders
Practice Questions
Enhanced Recovery After Colorectal Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
