Breast Surgery — MCQs
On this page
A 52 year old female underwent MRM (Modified Radical Mastectomy). After few years, she developed lymphedema of the ipsilateral arm. Which of the following malignancies can develop in her arm?
A 30 year old lady comes with history of bloody discharge from her right nipple while taking bath. On examination, there is a cystic swelling in the subareolar region. The clinical diagnosis would be:
Nottingham prognostic Index is used for:
Which of the following statements regarding lymphoedema following breast cancer treatment are correct? 1. Incidence has decreased due to rarely combined therapy of axillary LN dissection and radiotherapy 2. Precipitating cause like LN metastasis is a major determinant 3. The condition is often painful 4. Oedematous limb is susceptible to bacterial infection Select the correct answer using the code given below:
A 32-year-old woman presents with a 2 cm breast mass. Core needle biopsy shows invasive ductal carcinoma, ER+, PR+, HER2-. Sentinel lymph node biopsy reveals 2 positive nodes with no extracapsular extension. What is the most appropriate next step in management?
A 45-year-old woman with BRCA1 mutation has completed childbearing and requests prophylactic surgery. She has no evidence of breast or ovarian cancer. Her mother died of ovarian cancer at age 50, and her sister had breast cancer at age 35. Evaluate the optimal prophylactic surgical strategy.
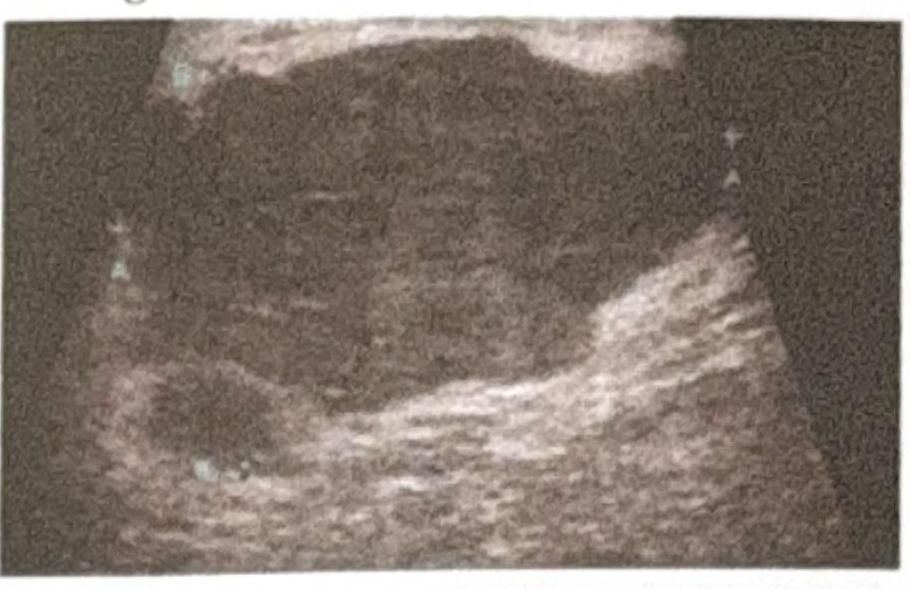
A patient presents to the OPD with a right-sided ulcerated breast lesion. Radiological imaging shows liver metastasis, as seen in the provided ultrasound image. What is the most appropriate management?
A patient presents with upper limb swelling after undergoing a modified radical mastectomy (MRM). What is the most likely cause?
Which of the following is not a relative contraindication for breast conservative surgery?
A 45-year-old woman with early-stage breast cancer is discussing treatment options with her surgeon. Which of the following statements regarding breast conservation surgery is NOT true?
Practice by Chapter
Breast Anatomy and Physiology
Practice Questions
Benign Breast Diseases
Practice Questions
Breast Cancer Screening
Practice Questions
Breast Cancer: Diagnosis and Staging
Practice Questions
Surgical Management of Breast Cancer
Practice Questions
Oncoplastic Breast Surgery
Practice Questions
Sentinel Lymph Node Biopsy
Practice Questions
Axillary Surgery
Practice Questions
Breast Reconstruction Techniques
Practice Questions
Male Breast Disorders
Practice Questions
Phyllodes Tumors
Practice Questions
Management of Ductal Carcinoma In Situ
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app