Axillary Surgery — MCQs

Sentinel lymph node biopsy in carcinoma breast is done if -
N3a TNM staging of head and neck tumors (AJCC 8th edition) shows:
Which of the following walls of axilla is formed by the surgical neck of humerus:
What is a late complication of elbow dislocation?
Axillary Nerve Injury is least likely in:
A patient with head and neck cancer has a contralateral lymph node of 3 cm size. What is the N staging?
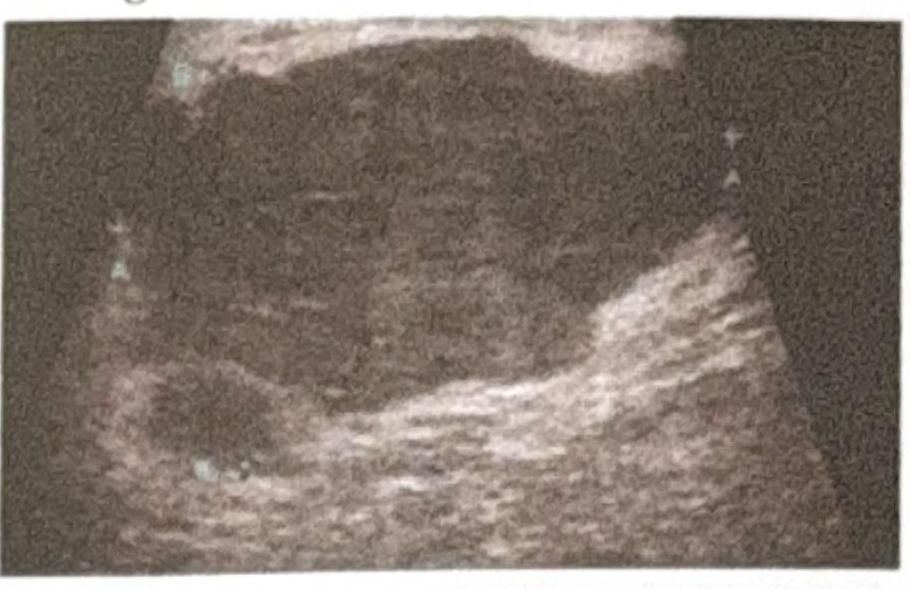
A patient presents to the OPD with a right-sided ulcerated breast lesion. Radiological imaging shows liver metastasis, as seen in the provided ultrasound image. What is the most appropriate management?
A 45-year-old woman with early-stage breast cancer is discussing treatment options with her surgeon. Which of the following statements regarding breast conservation surgery is NOT true?
Which of the following is a contraindication to breast conservation surgery?
In which of the following situations is breast conservation surgery not indicated?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
