Bariatric Surgery — MCQs

On this page
Which of the following local anesthetic agents is also a vasoconstrictor?
Which imaging modality is best for staging anal carcinoma?
What is the most appropriate cause for an increase in D-dimer levels noticed in the immediate post-operative period?
Which of the following is NOT true about bariatric surgery?
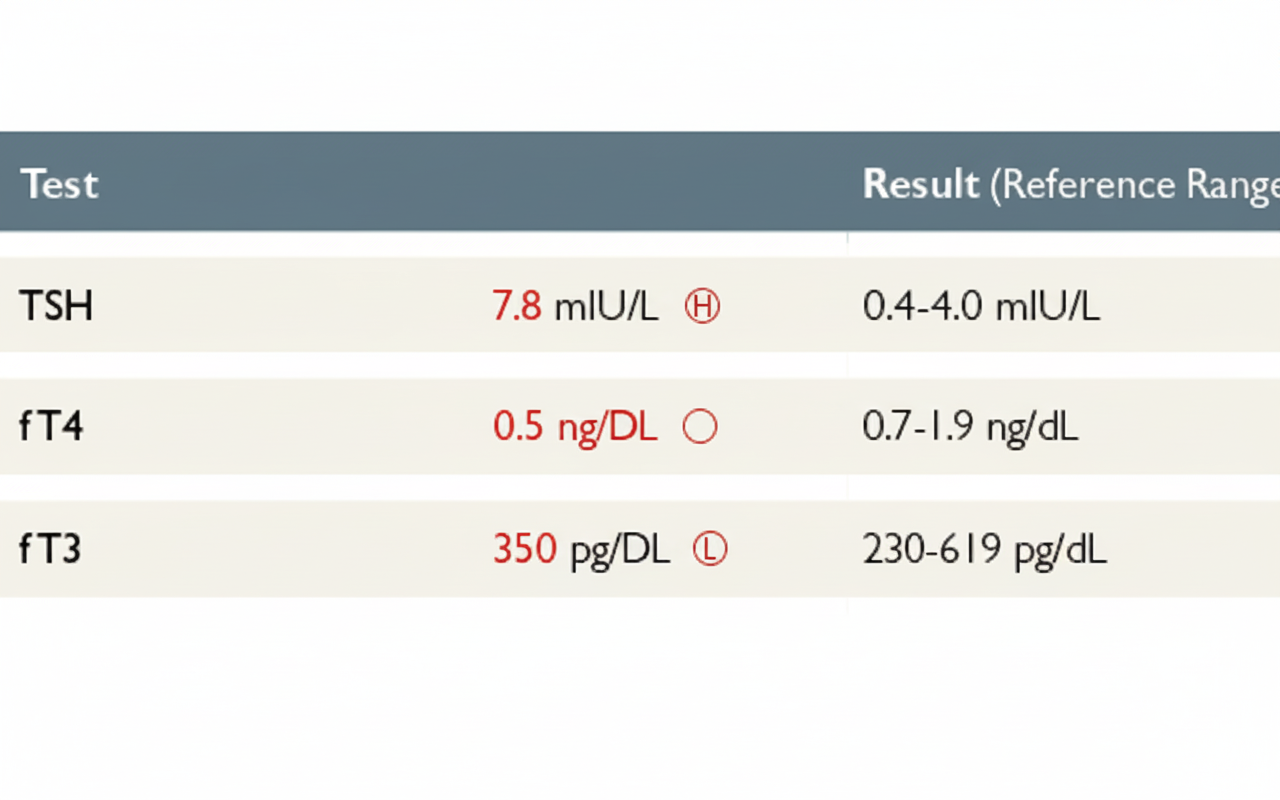
The laboratory investigation of a patient shows T4 and TSH levels. Which of the following is the most likely diagnosis?
In winter's WAR line, what does the Amber line represent?
All of the following regarding papillary carcinoma of the thyroid is true EXCEPT?
Which of the following is NOT a bariatric surgical procedure?
A 62-year-old woman with multiple myeloma is given pamidronate, a bisphosphonate. What is the proven benefit of this treatment?
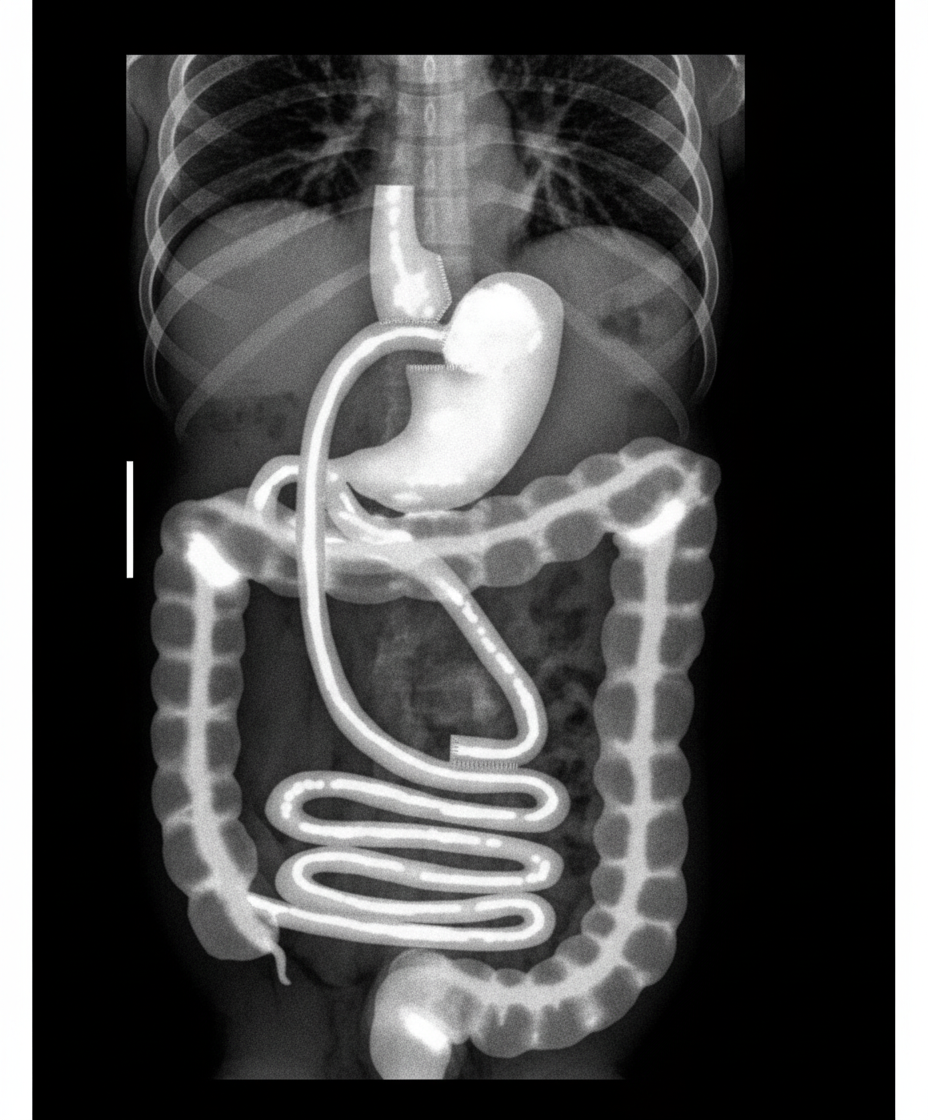
What procedure was most recently performed on this patient?
Practice by Chapter
Pathophysiology of Obesity
Practice Questions
Patient Selection and Preoperative Evaluation
Practice Questions
Restrictive Procedures
Practice Questions
Malabsorptive Procedures
Practice Questions
Sleeve Gastrectomy
Practice Questions
Roux-en-Y Gastric Bypass
Practice Questions
Biliopancreatic Diversion
Practice Questions
Adjustable Gastric Banding
Practice Questions
Revisional Bariatric Surgery
Practice Questions
Postoperative Management
Practice Questions
Nutritional Considerations
Practice Questions
Metabolic Effects of Bariatric Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
