Ultrasound — MCQs

On this page
Which embryonic structure, identified earliest on ultrasound, confirms pregnancy?
What does the "sea shore sign" on ultrasound indicate?
What is the most commonly used piezoelectric crystal?
A patient has a surgical cause of obstructive jaundice. Which of the following can Ultrasound NOT detect?
The double bleb sign on ultrasound is indicative of which of the following?
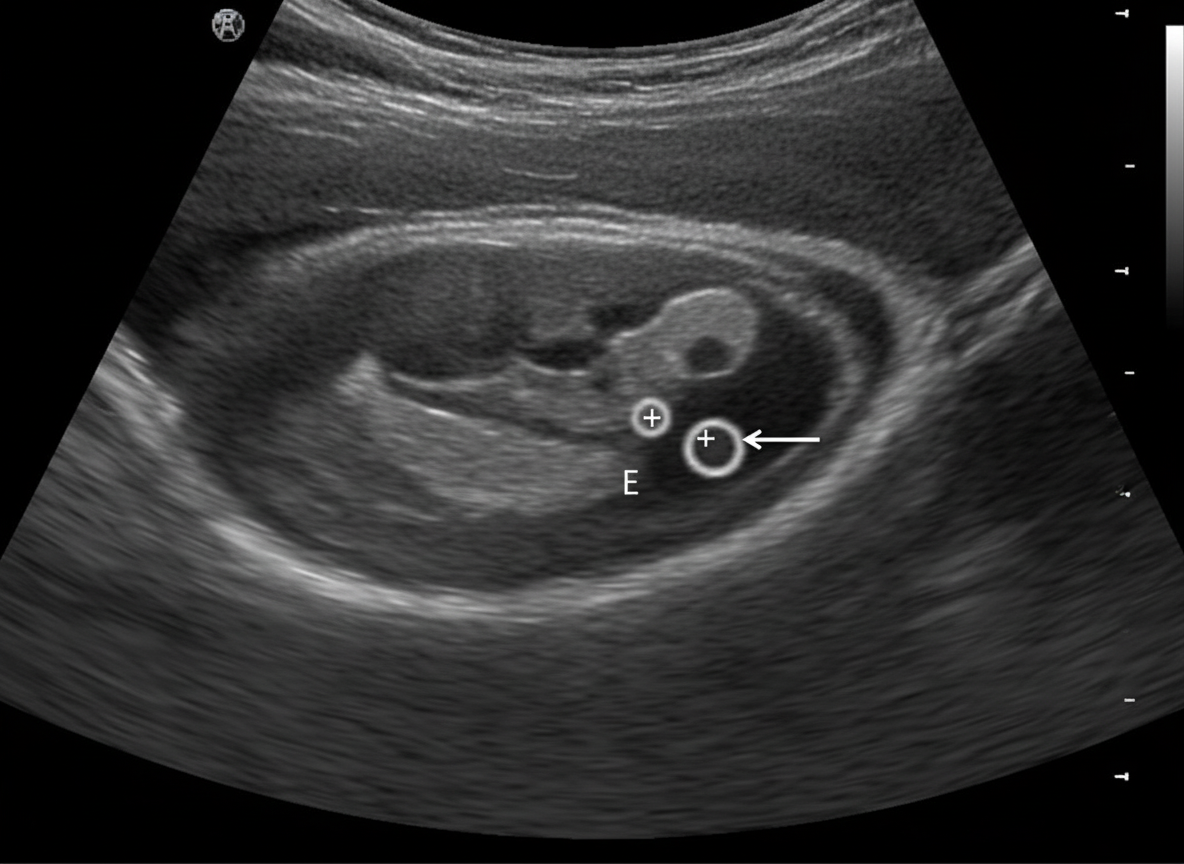
A sonogram demonstrates a Crown-Rump Length (CRL) of an 8-week fetus. The arrow in the image points to which of the following structures?
Which of the following imaging modalities is NOT included in the PI-RADS reporting scheme for prostate glands?
What is the investigation of choice to detect a 4 mm nodule in the pancreas?
Which of the following statements regarding Doppler ultrasound is incorrect?
Evaluation of cardiac valve motion and fetal heart rate is done in which mode of ultrasound?
Practice by Chapter
Physics of Ultrasound
Practice Questions
Instrumentation and Techniques
Practice Questions
Abdominal Ultrasonography
Practice Questions
Pelvic Ultrasonography
Practice Questions
Obstetric Ultrasonography
Practice Questions
Small Parts Ultrasonography
Practice Questions
Musculoskeletal Ultrasonography
Practice Questions
Vascular Ultrasonography
Practice Questions
Pediatric Ultrasonography
Practice Questions
Contrast-Enhanced Ultrasound
Practice Questions
Ultrasound-Guided Interventions
Practice Questions
Doppler Ultrasound Principles and Applications
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
