Ultrasound — MCQs

On this page
What is the frequency range of sound waves typically used for transabdominal ultrasonography?
Hyperchoice hepatic metastases on USG are seen in which of the following malignancies?
Which one of the following congenital malformations of the fetus can be diagnosed in the first trimester by ultrasound?
Comment on the provided ultrasound image?
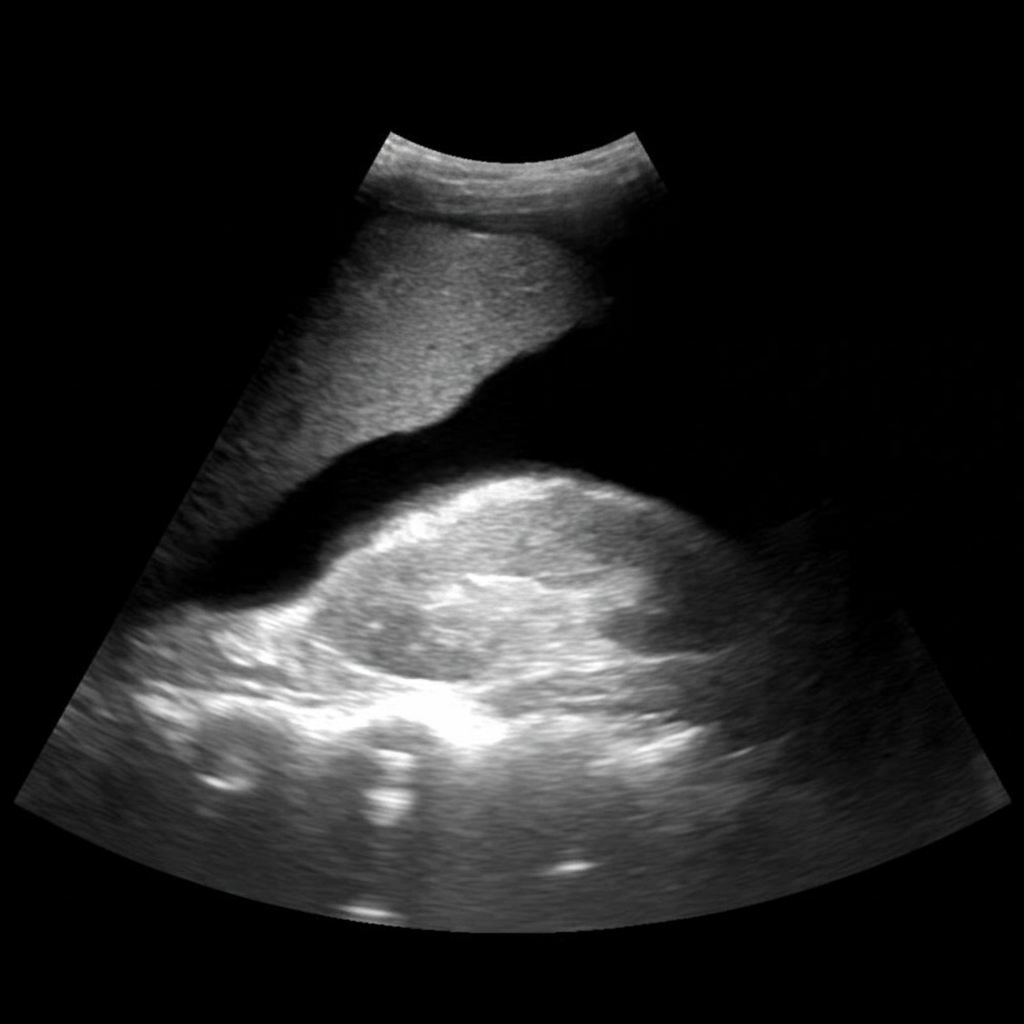
At what gestational age can ultrasound detect cardiac activity?
Which of the following probes is used for transcranial ultrasonography?
The twin peak sign is seen in which of the following conditions?
Time sector scanning of neonates is preferred because of which most practical reason?
What is the ultrasound frequency range typically used for diagnostic purposes in obstetrics?
T-sign is seen in which type of twin pregnancy?
Practice by Chapter
Physics of Ultrasound
Practice Questions
Instrumentation and Techniques
Practice Questions
Abdominal Ultrasonography
Practice Questions
Pelvic Ultrasonography
Practice Questions
Obstetric Ultrasonography
Practice Questions
Small Parts Ultrasonography
Practice Questions
Musculoskeletal Ultrasonography
Practice Questions
Vascular Ultrasonography
Practice Questions
Pediatric Ultrasonography
Practice Questions
Contrast-Enhanced Ultrasound
Practice Questions
Ultrasound-Guided Interventions
Practice Questions
Doppler Ultrasound Principles and Applications
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
