Musculoskeletal Ultrasonography — MCQs

Deltoid ligament is attached to all, except which structure?
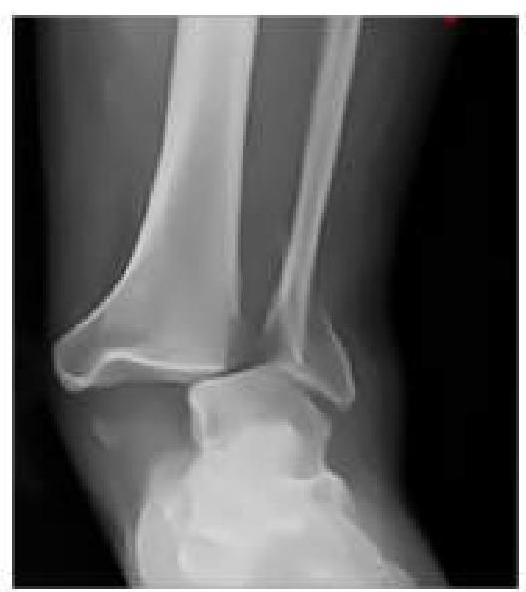
An RTA patient presented to the emergency department with severe pain in the ankle. An X-ray was performed, given below. What is the best next step in management?
Test shown in the video is for which structure & its nerve supply:
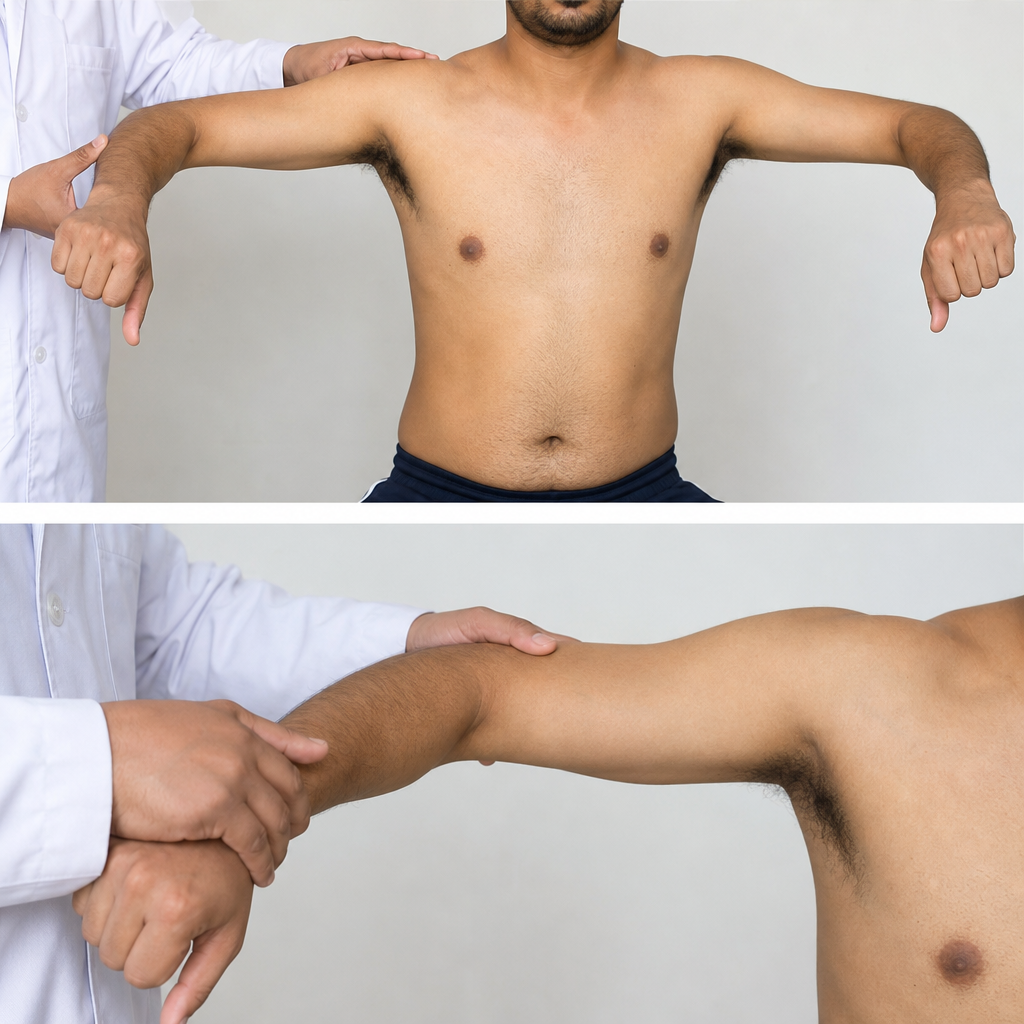
Rupture of extensor pollicis longus tendon occurs in all of the following except -
Which of the following is an intra-articular tendon?
In a child, non-functioning kidney is best diagnosed by
Transrectal ultrasonography in carcinoma prostate is most useful for –
Which is not echogenic while doing ultrasonography:
Which of the following ultrasound features of a thyroid nodule is not suggestive of malignancy?
Which of the following liver metastases appear hypoechoic on ultrasound?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
