Radiological Anatomy — MCQs

On this page
Which of the following can be most accurately identified on an X-ray?
For viewing the superior orbital fissure, what is the best radiographic view?
Which of the following radiographs is best for diagnosing a growth in the maxillary sinus?
What is the imaging study of choice for the paranasal sinuses?
Radiographically, the mental foramen lies between the roots of which teeth?
Which radiological view is best suited for examining fractures of the condylar neck of the mandible?
Which X-ray view is used to visualize the optic foramen?
Which of the following conditions or devices is generally considered safe for an MRI scan?
What is the primary basis for Magnetic Resonance Imaging (MRI)?
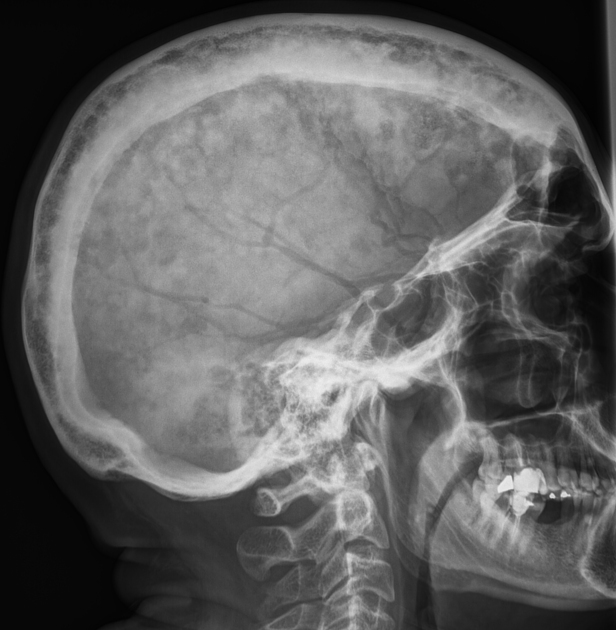
The following radiographs are most likely associated with which condition?
Practice by Chapter
Radiographic Anatomy of Skull and Face
Practice Questions
Radiographic Anatomy of Spine
Practice Questions
Radiographic Anatomy of Chest
Practice Questions
Radiographic Anatomy of Abdomen
Practice Questions
Radiographic Anatomy of Extremities
Practice Questions
Cross-sectional Anatomy: Brain and Head
Practice Questions
Cross-sectional Anatomy: Neck
Practice Questions
Cross-sectional Anatomy: Thorax
Practice Questions
Cross-sectional Anatomy: Abdomen and Pelvis
Practice Questions
Vascular Anatomy
Practice Questions
Developmental Anatomy Variations
Practice Questions
Anatomic Landmarks for Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
