Radiological Anatomy — MCQs

On this page
A 50-year-old male patient complains of facial heaviness, headache, and nasal congestion. He has a history of chronic sinusitis. A Waters view X-ray was performed. What is the typical positioning of the canthomeatal line relative to the film in this projection?
Thirteen pairs of ribs can be seen in all of the following conditions except?
The radiopacity of the zygoma is superimposed on the roots of which teeth?
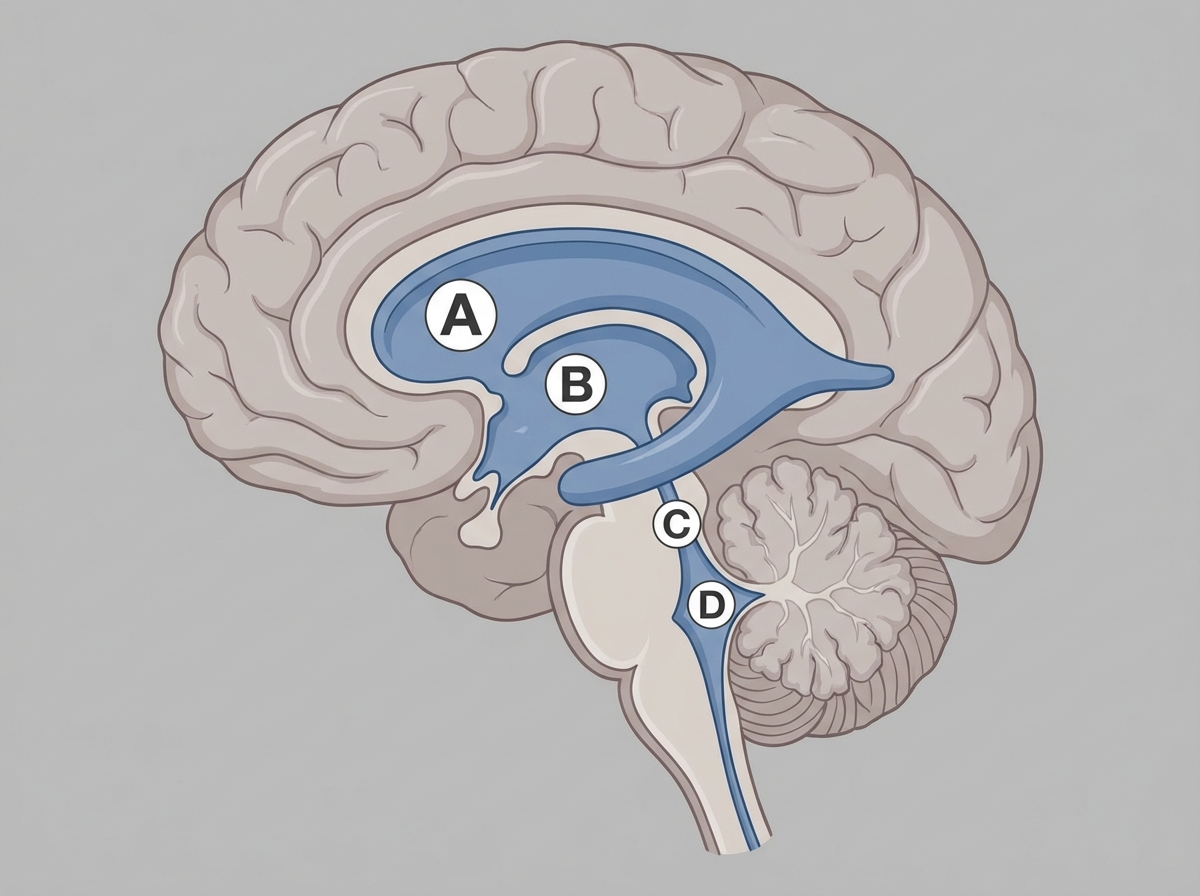
Cerebrospinal fluid is formed by the vascular choroid plexus in which structure?
What is the term for a thin radiolucent line that follows the outline of a tooth?
Which radiographic view best visualizes the C1 and C2 vertebrae?
A radiograph of a mandibular 3rd molar shows fading of trabeculations and narrowing of the canal in the apical region of the tooth. What is the diagnosis?
Which developmental cyst does not involve bone and may not be visible on radiographs, but causes swelling in the mucobuccal fold and the floor of the nose near the attachment of the ala over the maxilla?
Which of the following is NOT a radiological feature of scleroderma?
Which of the following does NOT contribute to the right side of the mediastinal shadow?
Practice by Chapter
Radiographic Anatomy of Skull and Face
Practice Questions
Radiographic Anatomy of Spine
Practice Questions
Radiographic Anatomy of Chest
Practice Questions
Radiographic Anatomy of Abdomen
Practice Questions
Radiographic Anatomy of Extremities
Practice Questions
Cross-sectional Anatomy: Brain and Head
Practice Questions
Cross-sectional Anatomy: Neck
Practice Questions
Cross-sectional Anatomy: Thorax
Practice Questions
Cross-sectional Anatomy: Abdomen and Pelvis
Practice Questions
Vascular Anatomy
Practice Questions
Developmental Anatomy Variations
Practice Questions
Anatomic Landmarks for Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
