Radiological Anatomy — MCQs

On this page
What is the most specific but late radiographic feature of scurvy?
What are dark radiolucent shadows appearing at the neck of teeth, most obvious on the mesial and distal aspect?
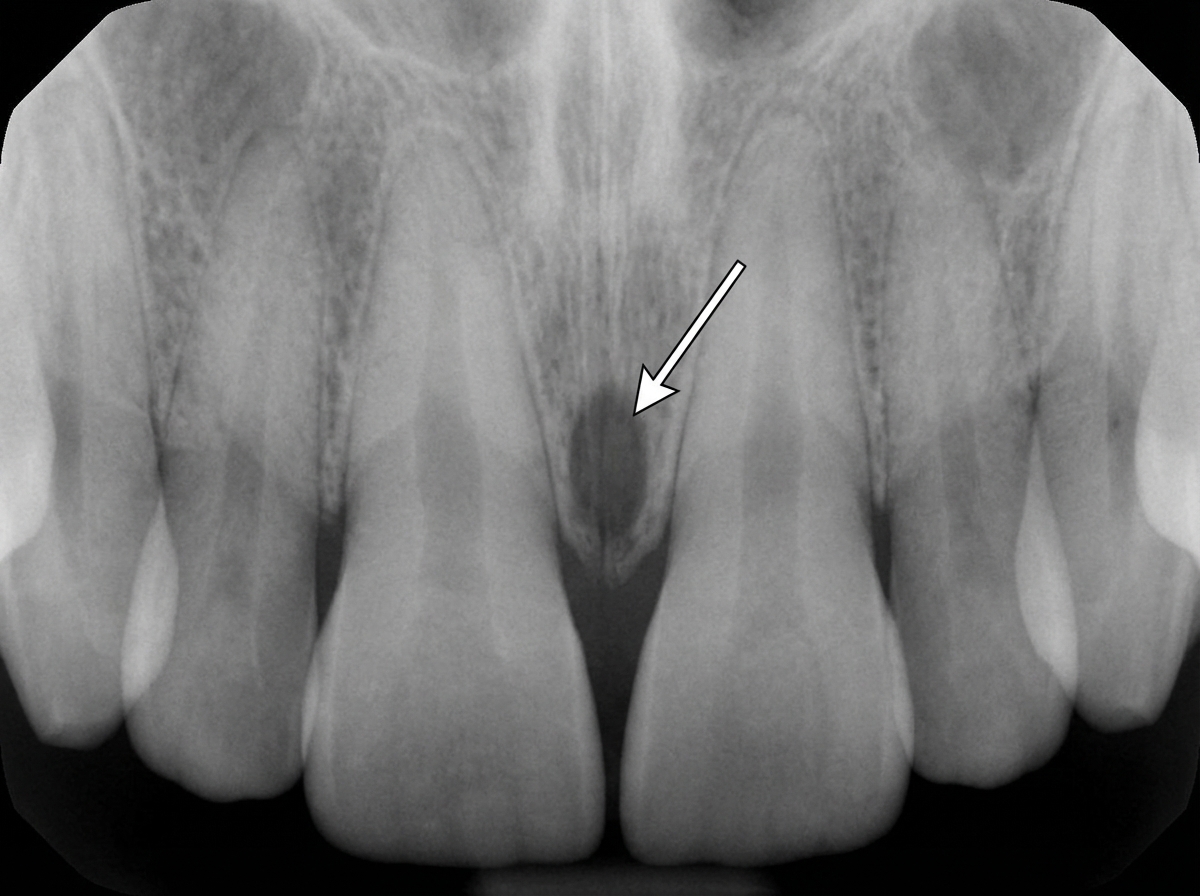
The structure marked with arrows is:
Waters view is best used for visualization of which sinus?
All of the following materials are radiopaque in nature except?
If the floor of the anatomic snuffbox and origin of the abductor pollicis brevis are damaged, which of the following bones is most likely to be involved?
On a routine radiographic exam, a well-defined radiolucent lesion was seen in the body of the mandible of a 17-year-old boy. At the time of operation, it proved to be an empty cavity. This is a(an) ____?
Which substance is most radiodense?
Which anatomical structure is best visualized on a periorbital view X-ray?
A "crew cut" appearance on skull X-ray is typically seen in which of the following conditions?
Practice by Chapter
Radiographic Anatomy of Skull and Face
Practice Questions
Radiographic Anatomy of Spine
Practice Questions
Radiographic Anatomy of Chest
Practice Questions
Radiographic Anatomy of Abdomen
Practice Questions
Radiographic Anatomy of Extremities
Practice Questions
Cross-sectional Anatomy: Brain and Head
Practice Questions
Cross-sectional Anatomy: Neck
Practice Questions
Cross-sectional Anatomy: Thorax
Practice Questions
Cross-sectional Anatomy: Abdomen and Pelvis
Practice Questions
Vascular Anatomy
Practice Questions
Developmental Anatomy Variations
Practice Questions
Anatomic Landmarks for Interventional Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
