Fractionation in Radiotherapy — MCQs

Fractional curettage is done in all except:
CHOP is used in the treatment of?
Which of the following is most radioresistant?
Principles used in Radio Therapy are:
A patient with cancer received an extreme degree of radiation toxicity. Further history revealed that the dose adjustment of a particular drug was missed during the course of radiotherapy. Which of the following drugs required a dose adjustment in that patient during radiotherapy to prevent radiation toxicity?
When is oxygen effective during radiotherapy?
What is the threshold radiation dose for the hematological syndrome?
Which of the following is NOT a radioprotector?
What is observed in the part of the bone which received radiotherapy?
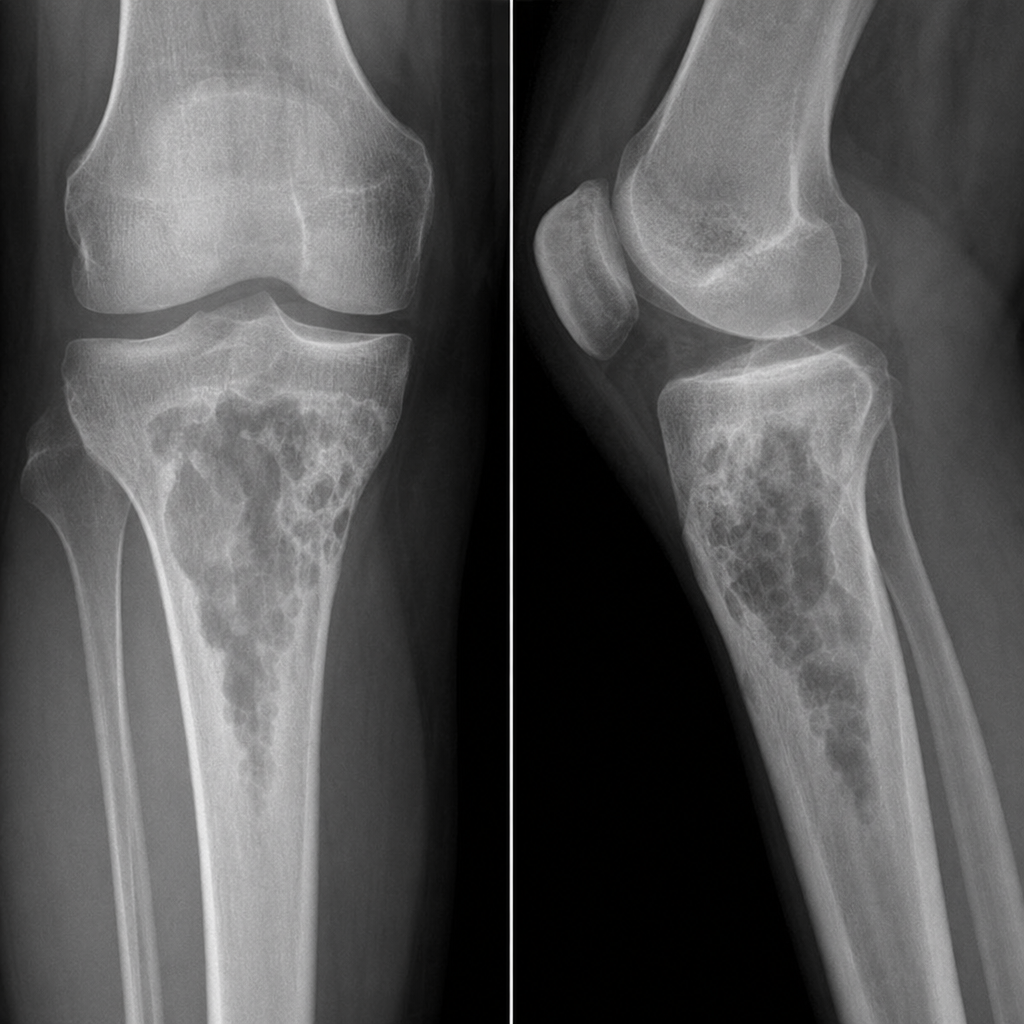
Which of the following statements about Linear Energy Transfer (LET) is true?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
