Radiation Physics and Protection — MCQs

On this page
What is the safest light to be used in a darkroom in an X-ray department?
Shields used in radiology are made up of what material?
Contrast in X-rays is dependent on which of the following factors?
All of the following have a naturally occurring decay product in a gaseous form, EXCEPT:
Amount of radioactivity absorbed by the body is measured by?
The overall degree of darkness of an exposed film is known as what?
Which of the following drugs is radioprotective?
The target of the X-ray tube is angulated to produce all the following effects, EXCEPT?
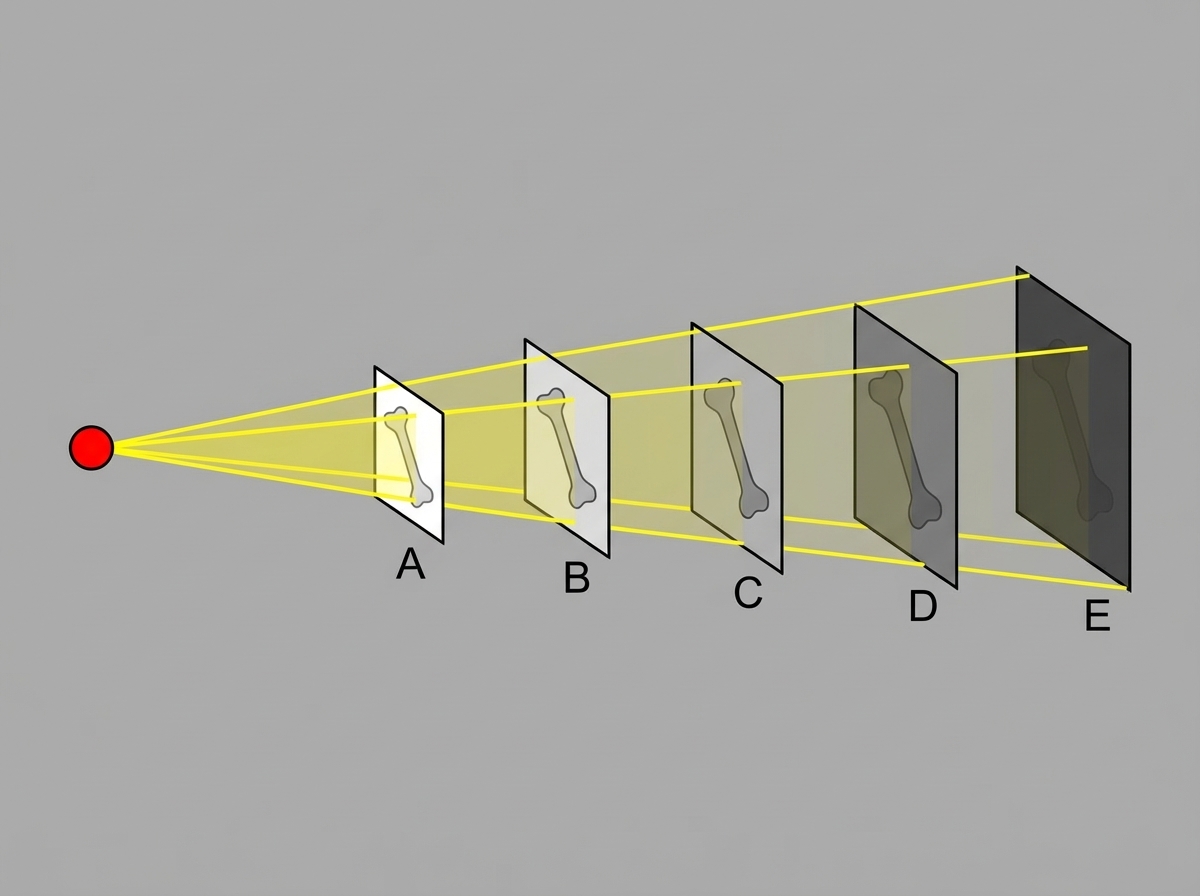
If the exposure of film A is R, then the exposure of film E is:
What is the conventional unit of Exposure?
Practice by Chapter
Electromagnetic Radiation
Practice Questions
X-ray Production
Practice Questions
Interaction of Radiation with Matter
Practice Questions
Radiation Measurement Units
Practice Questions
Radiation Detectors
Practice Questions
Radiobiology Fundamentals
Practice Questions
Radiation Protection Principles
Practice Questions
Personnel Monitoring
Practice Questions
Shielding Design and Calculations
Practice Questions
Radiation Dose Optimization
Practice Questions
Regulatory Requirements
Practice Questions
Radiation Accidents Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
