Radiation Physics and Protection — MCQs

On this page
Which investigation is contraindicated in pregnancy?
The following diagram shows production of X-rays. This is known as: (Recent NEET Pattern 2016-17)
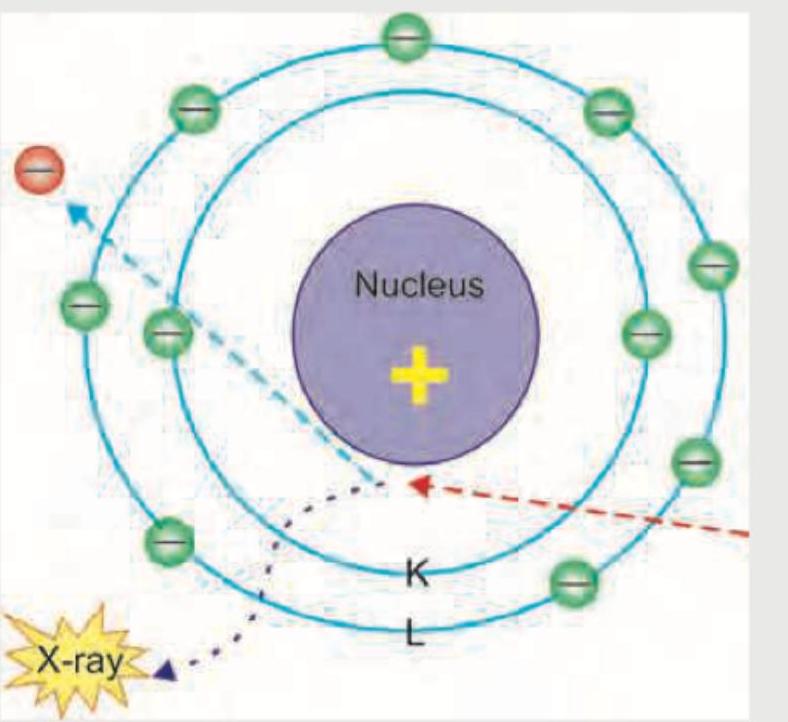
A radiopaque density may be noticed in poisoning by which of the following agents?
Identify the marked structure in the given image.
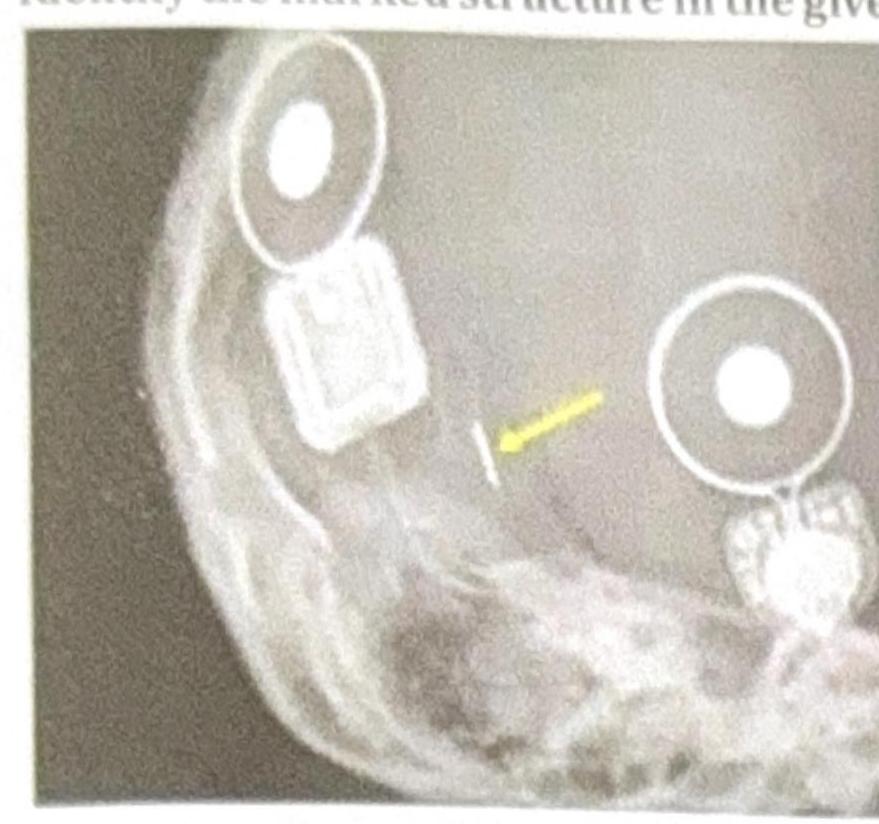
Which of the following typically results in the maximum radiation exposure?
Which of the following investigations work on the same principle?
A developer at high temperature will cause:
Which of the following reduces the development of unexposed Ag halide crystals, and also acts as an antifog agent?
At t = 0 there are 6 x 10^23 radioactive atoms of a substance, which decay with a disintegration constant (λ) equal to 0.01/sec. What would be the initial decay rate?
The longest half life is that of:
Practice by Chapter
Electromagnetic Radiation
Practice Questions
X-ray Production
Practice Questions
Interaction of Radiation with Matter
Practice Questions
Radiation Measurement Units
Practice Questions
Radiation Detectors
Practice Questions
Radiobiology Fundamentals
Practice Questions
Radiation Protection Principles
Practice Questions
Personnel Monitoring
Practice Questions
Shielding Design and Calculations
Practice Questions
Radiation Dose Optimization
Practice Questions
Regulatory Requirements
Practice Questions
Radiation Accidents Management
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
